A convex ostomy skin barrier can help prevent output leakage and skin issues. Unfortunately, some misconceptions about convexity may keep people with ostomies from using it.
A convex pouching system refers to the shape of the back of the ostomy skin barrier – the side that goes against your skin. A convex skin barrier is not flat, rather it is curved or dome shaped. Using an integrated convex skin barrier is often referred to as “adding convexity” to a pouching system. This convexity provides a gentle push on the belly, allowing the stoma to protrude up and outward. This can help output go directly into the pouch and not under the skin barrier (which can cause a leak).
Common reasons for using convexity are to prevent leakage and related skin issues, and to avoid having to change the pouching system more frequently. If your pouching routine or body weight has changed, chances are it’s time to consider using a convex skin barrier.

Flat Skin Barrier

Convex Skin Barrier
Below are a few myths or misconceptions about using convexity:
- All convexity is the same
Convexity should be chosen and customized based on your specific stoma and body shape. There are two main types of convexity: soft and firm. Soft convexity is flexible and conforms to your body as you move. Firm convexity is rigid and provides firm support around your stoma to help it stick out. In most cases, soft convex skin barriers are used on firmer abdomens, and firm convex skin barriers work best on softer abdomens. Someone may have a bad experience with convexity, only to learn that it was the wrong type for their stoma, body shape, or output. It’s important to know that the convex skin barrier opening needs to be close to the stoma in order to help the stoma protrude. This will also help reduce the possibility of leakage.
- A convex skin barrier is uncomfortable or even painful
If your convex skin barrier is causing pain or discomfort, you are not wearing the right type of convexity. Based on your needs, and with guidance from a healthcare professional, consider trying some of the many convex barrier options available and see if they make a difference. The importance of addressing leakage should outweigh the fear of trying something different. Use the health of the skin around your stoma as a barometer. If your skin looks good, and you are not leaking, you’ll know you’re using the right type of ostomy skin barrier for a good fit.
- I have to wait to use convexity
You don’t need to wait a certain amount of time before using a convex skin barrier. Each person is different. Some may need to add convexity immediately after surgery, while others may not need to add it at all. There is no concrete rule, and it depends on the type of stoma you have and how well it protrudes. If your belly is soft enough, you can start right away. Again, it’s important to prevent leakage while keeping the skin around your stoma healthy, and trying convexity could help accomplish both goals.
- If my stoma is level with my skin, I need a convex skin barrier
In most cases this is true, but choosing a type of convexity can depend on your stoma output. There are always exceptions and everyone has different experiences. For example, someone who has a colostomy with formed stool and regular bowel habits may not need to use convexity, even if their stoma is flush to the skin. That’s because formed stool is unlikely to leak underneath the skin barrier. On the other hand, more liquid output can increase the chances of leakage.
Consider trying a convex ostomy skin barrier to see if it will help prevent leakage and skin issues, and increase your pouching system wear time (i.e., how long you can wear your skin barrier before it fails). Convex skin barriers come in both pre-cut and cut-to-fit options and are covered by most insurance plans. An ostomy nurse can help determine which type of convexity is right for you and when you should use it.
For more information on skin barrier convexity and other resources, visit the Hollister Ostomy Learning Center.
Terri Cobb earned her RN degree in 1991 and became a board-certified CWOCN in 2011. Currently on staff at the Cleveland Clinic in Cleveland, Ohio, her responsibilities include caring for ostomy patients of all age groups from the neonate and beyond. Terri interacts with patients in all phases of their journey from pre-op, to immediate post-op and through follow-up care. Financial Disclosure: Terri received compensation from Hollister Incorporated for her contributions to this article.
Editor’s note: This article is from one of our digital sponsors, Hollister Incorporated. Sponsor support along with donations from readers like you help to maintain our website and the free trusted resources of UOAA, a 501(c)(3) nonprofit organization.




 The last day on the river was a half day. Once we got off the boats we are onto a bus for three hours. Luckily there was a real bathroom stop. Here I just switched out bags. We got back to the hotel and into the shower I went. I had so much adhesive on my skin. I used a ton of adhesive remover, then took a face cloth and washed the whole area. My skin looked pretty good for being engulfed in adhesive for 8 days lol. It took a while to get all the adhesive off. It felt amazing when it was. Obviously, when I got out of the shower I dried off and put on a new ring, wafer and bag, no brava strips. My skin was very happy for this.
The last day on the river was a half day. Once we got off the boats we are onto a bus for three hours. Luckily there was a real bathroom stop. Here I just switched out bags. We got back to the hotel and into the shower I went. I had so much adhesive on my skin. I used a ton of adhesive remover, then took a face cloth and washed the whole area. My skin looked pretty good for being engulfed in adhesive for 8 days lol. It took a while to get all the adhesive off. It felt amazing when it was. Obviously, when I got out of the shower I dried off and put on a new ring, wafer and bag, no brava strips. My skin was very happy for this. I was miserable. My family was miserable. But, I’d had enough and didn’t want any more treatments. Soon I was back in the hospital and one doctor reviewed ALL my info and said he knew exactly how to fix me…OK, just one more surgery then. Well, he was right…he fixed me!! I was no longer having incontinence issues, I could eat again (personalized diet plan) and was feeling great compared to the previous ten years. End of story right?!
I was miserable. My family was miserable. But, I’d had enough and didn’t want any more treatments. Soon I was back in the hospital and one doctor reviewed ALL my info and said he knew exactly how to fix me…OK, just one more surgery then. Well, he was right…he fixed me!! I was no longer having incontinence issues, I could eat again (personalized diet plan) and was feeling great compared to the previous ten years. End of story right?!
 Guess what? I didn’t win. I did not even place in the top 10. I went to the coronation party with a stage smile and promptly excused myself with my best friend by my side. She knew I needed to cry. As we reached the bottom of the grand staircase I could feel the tears of disappointment welling, and her hand grasping tighter to my arm letting me know I just had to keep it together for a few more seconds. At that moment a woman approached. She wanted to let me know her husband has an ostomy and seeing me on stage gave them so much hope and even though I didn’t win they were cheering for me! Again, I had to thank the universe for letting me know I was exactly where I was supposed to be.
Guess what? I didn’t win. I did not even place in the top 10. I went to the coronation party with a stage smile and promptly excused myself with my best friend by my side. She knew I needed to cry. As we reached the bottom of the grand staircase I could feel the tears of disappointment welling, and her hand grasping tighter to my arm letting me know I just had to keep it together for a few more seconds. At that moment a woman approached. She wanted to let me know her husband has an ostomy and seeing me on stage gave them so much hope and even though I didn’t win they were cheering for me! Again, I had to thank the universe for letting me know I was exactly where I was supposed to be.

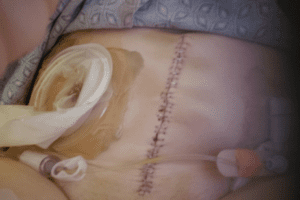 I was not in a great deal of pain which was easily managed with Tylenol. I was definitely weak, but otherwise ok. I went home in 4 days, on my own with my urostomy.
I was not in a great deal of pain which was easily managed with Tylenol. I was definitely weak, but otherwise ok. I went home in 4 days, on my own with my urostomy. Rudolph, my red, round stoma
Rudolph, my red, round stoma

 Night Drainage Pouch
Night Drainage Pouch






