Before my Inflammatory Bowel Disease (IBD) diagnosis at age 17, I always wanted to go to live events: concerts, listening parties, book signings, etc. But as a teen, I knew I held myself back. I didn’t want to look silly by showing up alone, and I’m extremely socially awkward. What if I say the wrong things? Even putting myself back in the thought process makes my skin crawl.
Post-diagnosis and at the beginning of my ostomy surgery process, some of my medical trauma began to manifest as not wanting to be alone. Combined with the social discomfort that fluctuates with an ostomy, like apprehension around leaks, clogged filters, and farts, I created the perfect recipe for opting out of things if I didn’t have a companion.
The summer of 2022 changed things.
I remember being extremely low mentally, in pain, and constantly in and out of the hospital due to a fistula that my doctors hadn’t been able to detect on scans. In that period of isolation, rumination, and reflection, I made a promise to myself that if I ever felt better, I’d take advantage of it and figure out ways to do the things I’ve always wanted to do.
When I was finally healed and ready, I was excited to enjoy some live events, but that didn’t stop the fear and anxiety.
What if I had an emergency? What if I didn’t bring enough ostomy supplies? What if I couldn’t contact my family if I needed them?
I wanted to be safe and really listen to my body. I knew the only way I’d enjoy the experience was if I felt safe and prepared.
Here are some things I find myself consistently doing before, during, and after events that increase my comfort.
My Top Tips for Going Out with IBD or an Ostomy
1. Plan Ahead & Ask Questions
Before making any plans, I have conversations with my medical team and family. Often, they give me insight, reassure me I am physically ok to do certain things, and help me find out more information.
- ADA Accommodations: I reach out to venues & organizers for ADA (Americans with Disabilities Act) accommodations to have plans & contacts in place if I’m not feeling the best.
- ADA accommodations can look like:
- Medical/bigger bag allowance
- Safe snacks & water from home
- Priority access to seated spaces
- Chairs while waiting in line
- & more! I’m still discovering them myself!
- ADA accommodations can look like:
- Safe Foods: I look into food venues and menus to make sure there are safe options for my IBD and ostomy-friendly eats.
- To avoid gas/cramping/bloating, I generally don’t eat lots of candy, fried/breaded foods, and carbonated beverages.
- Raw fruits, veggies, popcorn & nuts, if it’s during the morning & I’m not returning home/to my hotel for an extended period.
- I don’t consume alcohol at all.
- Bathroom Access: You can map out restrooms when you get to the venue, but if you can find a venue map online, bathrooms should be listed! Having an official bathroom access card from an IBD or ostomy organization like UOAA is helpful, too!
It’s also always nice to have names to reference staff members you’ve been in communication with, especially to build relationships if this is a place you’ll be frequenting. Repeating this process helped build the foundation of my concert review series on social media!
2. Bring What You Need
I’ve made several videos documenting what I keep in my concert bag, but I’m never leaving without:
- Supplies to do at least one ostomy bag change, including a fresh pouch, a barrier, adhesive remover spray, and deodorant
- Hydration drops
- Pill container
- Portable charger
- Wireless earbuds
The earbuds may seem a little odd because they’re not medically related, but in a crowded, noisy area, or if your hands are full, it’s always nice to just pop an earbud in to make a call. Depending on the temperature and venue rules, I also alternate between a handheld fan and hand warmers.
3. Listen To Your Body
For me, having an ostomy didn’t completely resolve my symptoms or “cure” my IBD. While I completely support research that recommends surgeries that may leave patients with a temporary ostomy and increase remission outcomes, I don’t support surgery being described as “the cure.”
Extraintestinal manifestations or “non-gut related symptoms” can still occur, most of which I’m still managing with a combination of medications and mental and physical therapies.
Fatigue, joint aches, dehydration, etc., are all common with IBD, and I’ve learned that a lot of the “prep” happens long before you decide to go somewhere.
- Dehydration: Hydrate, hydrate, hydrate. I know it’s annoying to hear it, but I always feel better if I’m properly hydrated.
- Joint Aches: If there’s prolonged standing, walking, or sitting, I’m usually opting for some type of compression support on my hands, legs, and arches of my feet to combat any swelling or irritation.
- Fatigue: Getting enough rest before and after solo activities helps with recovery! Generally, I’m taking things slow 1-2 days before and after each event to support my body as much as possible.
These tips are general, but they aren’t one-size-fits-all. Tweak things to your personal needs and don’t feel bad if you make a few mistakes along the way; you’re human! You should always consult your doctors if you have any questions about anything that could affect your treatment or health.
Embracing solo activities isn’t about being alone constantly. Years into this process, I’ve met some of the coolest people during my solo adventures, and I’m so thankful that I’m working towards being comfortable with just myself.
Having self-confidence that helps strengthen this type of exploration still doesn’t always come naturally to me as someone with IBD and a permanent ostomy, but I feel a lot better knowing I’m prepared!
Kaylaa’ is a Coloplast product user who received compensation from Coloplast to provide this information. Each person’s situation is unique, so your experience may not be the same. Talk to your healthcare professional about which product might be right for you.
Coloplast develops products and services that make life easier for people with intimate healthcare needs. Working closely with the people who use our products, we create solutions that are sensitive to their special needs. Our business includes ostomy care, continence care, advanced wound care, interventional urology, and voice & respiratory care.
Follow Coloplast on Instagram, Facebook, and YouTube, or visit us online at https://www.coloplast.us/
Editor’s note: This blog is from a UOAA digital sponsor, Coloplast. Sponsor support along with donations from readers like you help to maintain our website and the free trusted resources of UOAA, a 501(c)(3) nonprofit organization.


 As you recover, if you have a descending or sigmoid colostomy you may want to ask your doctor or ostomy nurse if you are a candidate for
As you recover, if you have a descending or sigmoid colostomy you may want to ask your doctor or ostomy nurse if you are a candidate for 
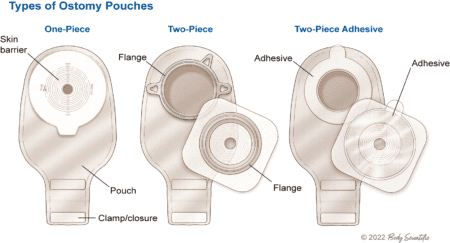
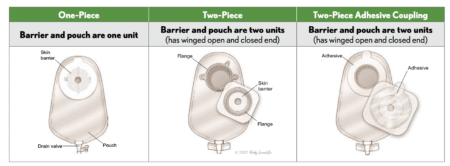
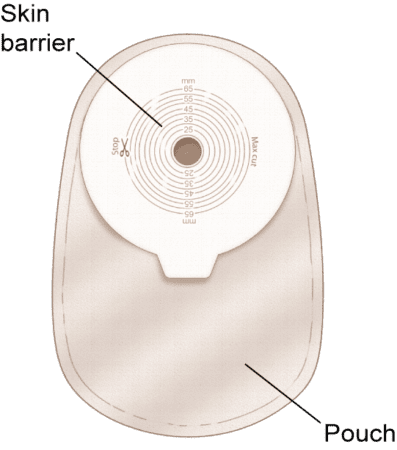
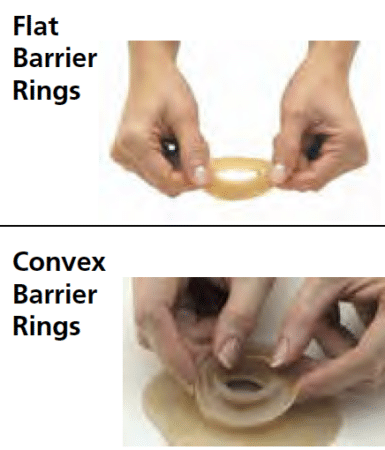 Picking the best skin barrier is critical since it protects the skin around the stoma and enables a secure seal and fit. Your choice depends on your stoma, output, and other factors, such as sensitivity. Frequent changers may ask about gentle adhesion options while those with liquid output may require a stronger adhesion. If your stoma size is changing or oval you may want to get cut-to-fit or moldable skin barriers while, if it is stable and round, pre-sized are a convenient option.
Picking the best skin barrier is critical since it protects the skin around the stoma and enables a secure seal and fit. Your choice depends on your stoma, output, and other factors, such as sensitivity. Frequent changers may ask about gentle adhesion options while those with liquid output may require a stronger adhesion. If your stoma size is changing or oval you may want to get cut-to-fit or moldable skin barriers while, if it is stable and round, pre-sized are a convenient option.




