Colleen Reddington’s Ostomy Story
I’m interested in sharing my story because I know I am lucky to have a smart nurse practitioner for a sister who has advocated for me and helps me advocate for myself. When I was researching and looking for patients who had experienced the same non-cosmetic abdominal plastic surgery as I had, I was only able to find one person in the US. It has been so life-changing for me and I think others may benefit from it as well.
I was diagnosed with stage IIa rectal cancer in August 2019 after my baseline screening colonoscopy at 50. I wasn’t surprised; I knew something wasn’t quite right and hadn’t been for a while. That fall I underwent radiation treatment and oral chemotherapy in preparation for Low Anterior Resection surgery in January 2020.
My tumor was removed along with about 80% of my rectum and 13 lymph nodes. I had clear margins and a temporary ileostomy. I had a distinctly unfortunate ileostomy situation – I also live with epilepsy and I wasn’t immediately aware that the ileostomy was spitting out most of my epilepsy meds before they could metabolize into my system. As a result, I had six tonic clonic seizures in six weeks (usually I have one or two a year) and I was a bit of a mess. Add in severe skin breakdown due to seal problems and there was no way I could start cleanup chemo. We decided to reverse the ileostomy earlier than expected, after just 8 weeks, at the end of March 2020.
This has been nothing short of life-changing. Prior to this surgery, I had so much difficulty getting a good seal that I dared not even shower with the appliance on.
I started what was supposed to be eight rounds of chemo in May. After two rounds I discovered I had a rectovaginal fistula. I opted to push through and deal with it later. As it was I had yet to regain bowel control and was dealing with many of the issues of LARS (Low Anterior Resection Syndrome).
I made it through four rounds of chemo before I was hospitalized for severe constipation. We decided I’d gotten all the good I was going to get from chemo and made plans to have surgery for a temporary colostomy in preparation for surgery to repair the rectovaginal fistula. The colostomy diverts everything, giving that area a break and hopefully ensuring greater success in repairing the fistula. Because the colostomy helped and in light of the incredibly high rate of recurrence for rectovaginal fistulas, I decided to keep it and pass on the fistula repair surgery.
But an interesting thing happened – when I got the colostomy my quality of life really improved! I no longer needed to wear a diaper. As time went on, I was still dealing with severe skin breakdown and problems getting a good seal. I have been overweight all my life and the fact my belly was soft with dips and valleys didn’t help. Additionally, because of carrying so much weight in my belly my colorectal surgeon was limited in the length of gut he had to work with and the stoma profile he was able to create.
My sister Madonna is a nurse practitioner and she suggested that I consult with a plastic surgeon to work with my colorectal surgeon. She thought perhaps they could do a panniculectomy and stoma re-site to give me a better landscape to work with. My colorectal surgeon had not done this before.
To make it even more unique, my sister was the charge nurse on the med/surg unit when my colorectal surgeon was doing his residency over 20 years ago. She already had a plastic surgeon in mind (one she had sent her patients to) so when I approached my colorectal surgeon with this possible solution to my seal/skin issues he trusted her judgment and agreed to it.
Unfortunately, due to the pandemic my surgery was delayed twice. I had it in March 2022, almost a year after I initiated the process.
This has been nothing short of life-changing. Prior to this surgery, I had so much difficulty getting a good seal that I dared not even shower with the appliance on. I used so many extra products and changed it out at least twice a week. Now, I use just the flange and it lasts all week – even through being in the pool five days a week, some days twice; through showers after every pool session.
I do have a parastomal hernia that my colorectal surgeon minimally repaired while re-siting but getting rid of the excess belly fat has even helped with managing that. I feel like I have my life back, without the anxiety, stress, and physical pain of a low-profile stoma and inadequate seal can cause.
Prior to this surgery, my stoma was placed almost parallel to my belly button which added to the trouble. The panniculectomy removed 10 pounds of belly fat and my bellybutton too. The surgery is not done for cosmetic reasons so some of the steps a plastic surgeon will take in doing a tummy tuck (like preserving the bellybutton) are not done in a panniculectomy.
Even with the seal/skin problems, I’ve always been grateful for my colostomy. But now I feel like my colostomy is really doing what it’s meant to do – helping me be in control and do whatever I want to do.
I have the option to reverse my colostomy at any time, but I won’t – it essentially takes care of the rectovaginal fistula (which remains stable since getting the colostomy) and also gives me bowel control, which I never regained after my temporary ileostomy reversal. I realize it wasn’t a long time but with only 20% of my rectum remaining, I’m not confident I ever would.
In addition to my water aerobics routine (I go M – F every morning and again in the afternoon three or four days for a total of 8 – 9 hours per week). I now shower also multiple times a day. I couldn’t do that before – I was only able to shower twice a week (when I changed my appliance) and resorted to sponge baths the rest of the time. Before, in addition to the flange and pouch, I used stoma powder, paste, and strips. Now I just need the flange and pouch and it gets me through a week. I’m saving money and creating less garbage. I’m also saving time. I used to have to let my flange “cure” for an hour before moving; now it takes about five minutes and I’m up and about.
Even with the seal/skin problems, I’ve always been grateful for my colostomy. But now I feel like my colostomy is really doing what it’s meant to do – helping me be in control and do whatever I want to do.

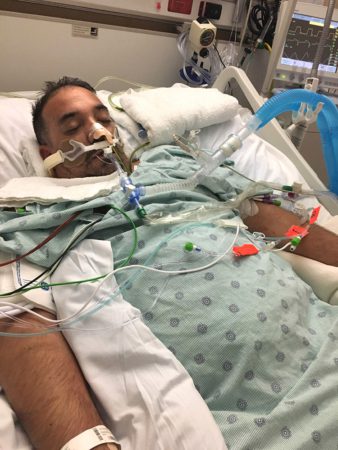 how they are doing and to never forget that they are going through similar things,” Gonzalez says. He received 12 sessions of chemotherapy for six months. While in the hospital for treatment during the Christmas Holiday Gonzalez, who is an advocate and speaker for father engagement in K through 12 education and active in several area PTA’s where he raised two children, had an idea to bring some cheer to fellow patients by having local children draw cards of support to his fellow patients.
how they are doing and to never forget that they are going through similar things,” Gonzalez says. He received 12 sessions of chemotherapy for six months. While in the hospital for treatment during the Christmas Holiday Gonzalez, who is an advocate and speaker for father engagement in K through 12 education and active in several area PTA’s where he raised two children, had an idea to bring some cheer to fellow patients by having local children draw cards of support to his fellow patients.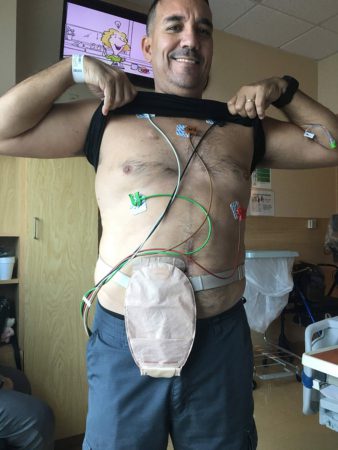 On June 25, 2021, he was taken off the TPN and underwent a successful reversal surgery to repair his intestines, clean up scar tissue, and remove the stoma.
On June 25, 2021, he was taken off the TPN and underwent a successful reversal surgery to repair his intestines, clean up scar tissue, and remove the stoma. Exercising with an Ostomy
Exercising with an Ostomy Some people wonder how they can ever find something positive in something so scary as an ostomy, but it can be done. You don’t need to do it in big
Some people wonder how they can ever find something positive in something so scary as an ostomy, but it can be done. You don’t need to do it in big 
 Every individual person’s disease treatment is unique but ostomy surgery for colorectal cancer may mean a temporary
Every individual person’s disease treatment is unique but ostomy surgery for colorectal cancer may mean a temporary 
 pantyliners in my underwear. When I retired from active duty in August 1996, I immediately started my second career as an Army JROTC Instructor in Bennettsville SC. I continued to go to the bathroom quite frequently and in the spring of the following year my daughter, who was six at the time, wanted me to play horsey with her and take her around the block. I bent down half in tears and told her that “daddy can’t play horsey because he is too sore on his bottom”. I immediately went to talk to my wife and we both agreed it was time to get back to having an ostomy bag. That summer at the Columbia SC Veterans Administration hospital, I had my third surgery to restore my ostomy due to my poor quality of life with the J Pouch. On the positive side, since I’ve had an external pouch, the veteran’s administration awarded me 100% total and permanent disability. I spent the next 23 years as an Army JROTC Instructor.
pantyliners in my underwear. When I retired from active duty in August 1996, I immediately started my second career as an Army JROTC Instructor in Bennettsville SC. I continued to go to the bathroom quite frequently and in the spring of the following year my daughter, who was six at the time, wanted me to play horsey with her and take her around the block. I bent down half in tears and told her that “daddy can’t play horsey because he is too sore on his bottom”. I immediately went to talk to my wife and we both agreed it was time to get back to having an ostomy bag. That summer at the Columbia SC Veterans Administration hospital, I had my third surgery to restore my ostomy due to my poor quality of life with the J Pouch. On the positive side, since I’ve had an external pouch, the veteran’s administration awarded me 100% total and permanent disability. I spent the next 23 years as an Army JROTC Instructor.
 Without an
Without an 


