Choosing an ostomy pouching system is a personal decision based on your stoma, your skin, your output (stool or urine), and your day-to-day routine. This guide breaks down the main types of ostomy pouching systems for colostomy, ileostomy, and urostomy, plus common skin barrier (wafer) options and accessories that can help prevent leaks and protect peristomal skin.
Quick overview: the main options
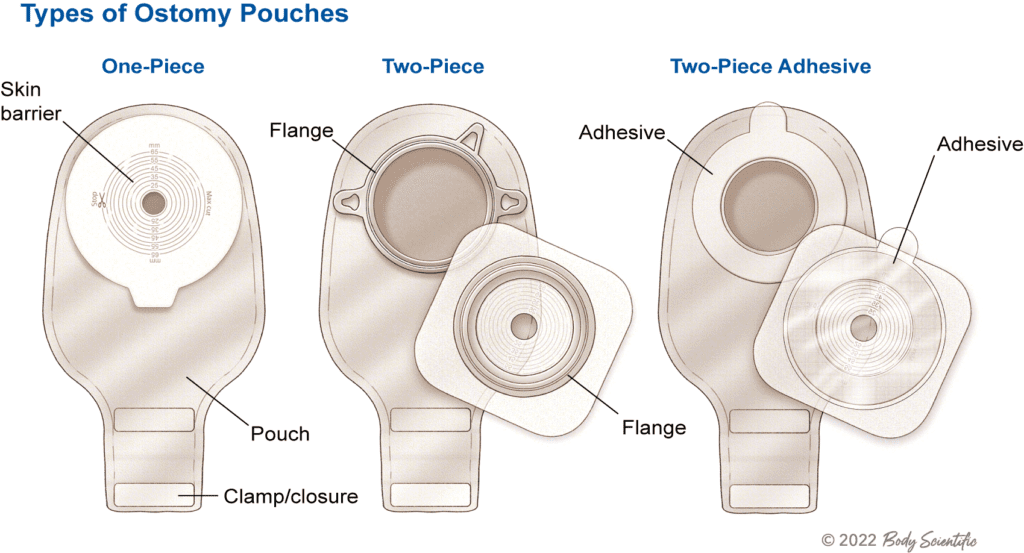
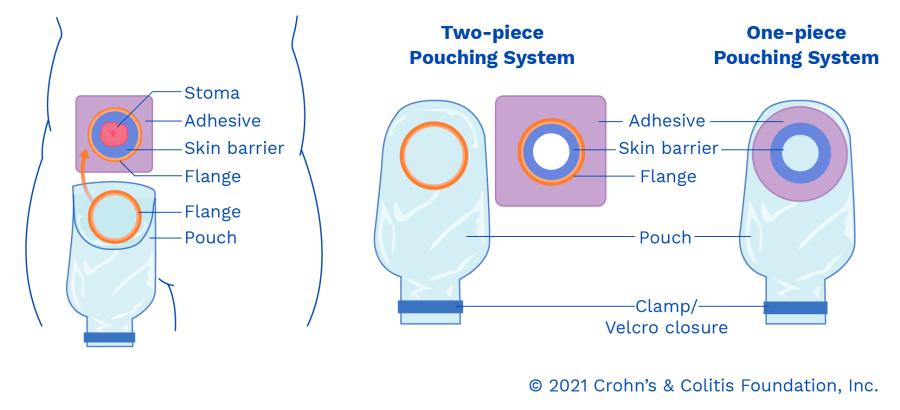
- Most pouching systems combine two essentials:
- Skin barrier (wafer): adheres to the skin around the stoma to create a seal
- Pouch: collects output
From there, pouching systems typically vary by:
- One-piece vs. two-piece design
- Drainable vs. closed-end pouches
- Flat vs. convex barriers
- Standard-wear vs. extended-wear materials
Drainable vs. closed-end pouches (colostomy & ileostomy)
Colostomy and ileostomy pouches are commonly available in two styles:
1. Drainable (open-ended) pouches
- Open at the bottom and emptied while still attached
- Usually closed with a tail closure (clip or integrated closure, depending on product)
2. Closed-end pouches
- Sealed at the bottom and typically discarded after one use
- Often preferred by people who have more predictable output patterns or who irrigate (where appropriate)
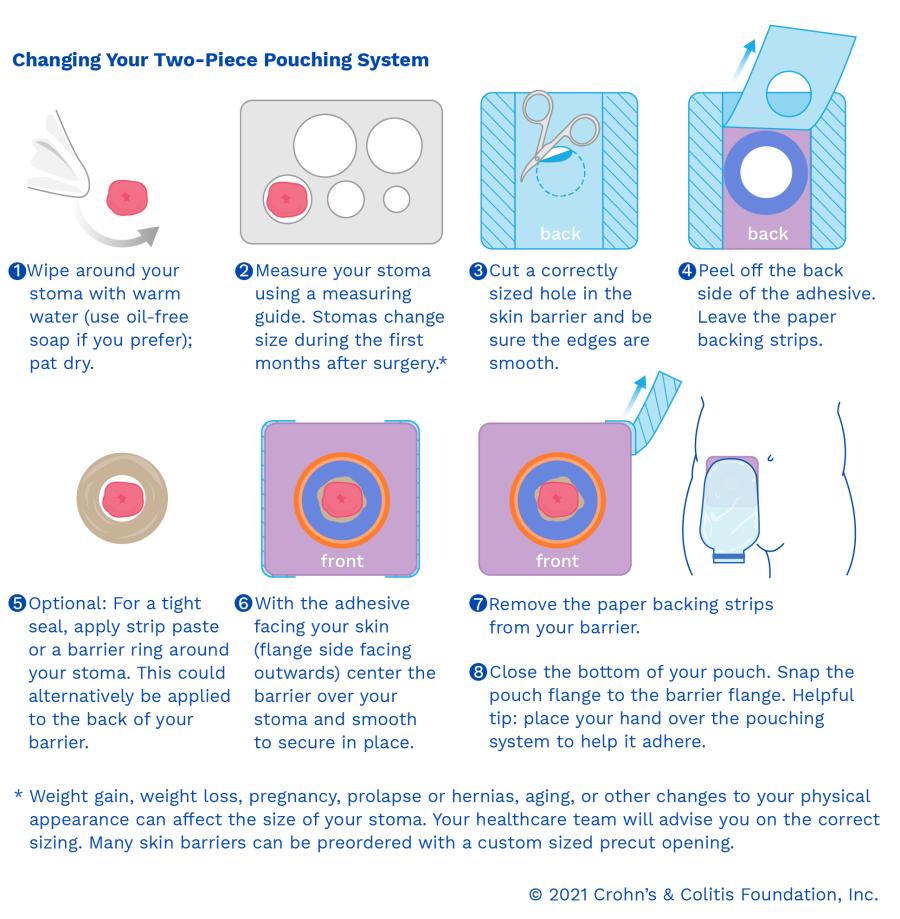
Two-piece ostomy pouching systems
A two-piece system lets you change the pouch while keeping the skin barrier/wafer in place. The pouch attaches to the barrier through a flange/coupling (often a snap-style ring connection).
United Ostomy Associations of America
Why people like two-piece systems
- Easier pouch changes without removing the barrier every time
- Flexibility to switch pouch styles (for example, different sizes or drainable vs. closed) while keeping the same barrier
Things to consider
- Some people find the coupling feels bulkier under clothing
- You’ll want to ensure the flange connection is secure and compatible with the matching barrier size
One-piece ostomy pouching systems
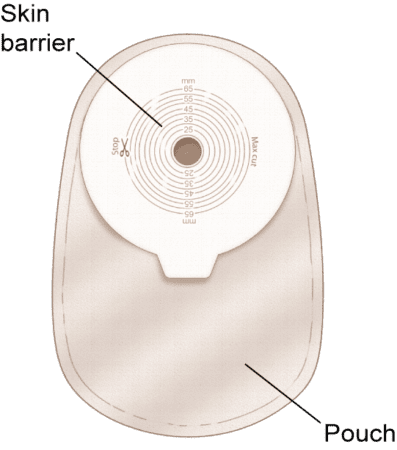
Colostomy Pouch One-Piece Closed End
A one-piece system combines the skin barrier/wafer and pouch into a single unit. This can feel simpler because there’s no coupling step — but when you change the pouch, you change the whole system (barrier included).
Why people like one-piece systems
- Simple, all-in-one application
- Often lower-profile because there’s no flange ring connection
Things to consider
- A full change includes removing and replacing the barrier, which may matter if your skin is sensitive.
Both one-piece and two-piece pouches may be either drainable or closed.
Irrigation systems (for some colostomies)
Some people with a colostomy may be able to irrigate, a process similar to an enema that helps empty stool from the colon through the stoma. Irrigation uses a specialized setup such as an irrigation bag, tubing/catheter, a stoma cone, and an irrigation sleeve (and sometimes lubricant).
After irrigation, some people choose a stoma cap or a small covering system instead of wearing a full pouch—when appropriate for their situation and clinician guidance.
Urinary pouching systems (urostomy)
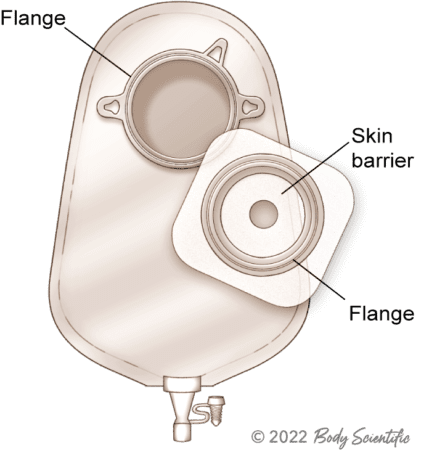
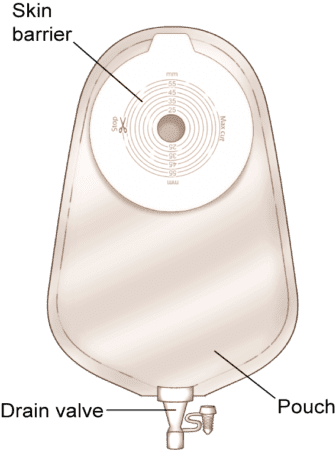
Urostomy pouching systems may be one-piece or two-piece, but they include features designed specifically for urine output, such as a drain valve/spout and options to connect to a leg bag or night drainage setup.
Styles and fit options (barriers, materials, and openings)
Beyond the major types above, pouching systems come in many styles to match different bodies and stomas:
Skin barrier shape
- Flat barriers sit level on the skin
- Convex barriers curve inward to help support a more secure seal for certain stoma/skin contours
Wear time materials
- Standard-wear or extended-wear materials (varies by product and output type)
- Flexibility and adhesive options
- Rigid vs. flexible barriers
- With or without adhesive backing
- With or without tape border
Stoma opening
- Pre-cut openings
- Cut-to-fit openings
Bottom closure
- Some drainable pouches include an integrated tail closure rather than a separate clip
Bottom line: there’s no single “right” pouching system. Many people try a few options (often using free samples) before landing on what fits best. If you’re dealing with leaks, discomfort, or skin irritation, it’s worth talking with an ostomy nurse or healthcare provider about adjustments.
Types of ostomy accessories
Accessories can improve comfort, seal, and skin protection. Here are common options:
Convex inserts
Convex-shaped plastic discs that insert inside the flange of certain two-piece products to add convexity and support. Some rings or strips can also be used to create added convexity.
Skin barrier paste, rings, and strips
Used to smooth skin folds/irregularities and fill gaps between the stoma and barrier, which may reduce leaks and improve wear time.
Important: ostomy paste is a caulking material — not an adhesive — and too much can reduce adherence.
Ostomy belts
Belts wrap around the abdomen and attach to loops on certain pouches. They can help support the pouch and may help maintain a seal (especially with convex barriers) or reduce reliance on adhesives if skin issues develop.
Pouch covers
Fabric covers that add comfort and help protect skin. Many modern pouches include built-in cloth covers on one or both sides.
Skin barrier wipes/liquid/powder
Often used when peristomal skin is irritated, moist, or weepy. Powders can support healing (remove excess), and liquid film barriers can help seal and protect skin before applying the barrier.
Tapes
Used to reinforce edges of the wafer/flange (faceplate) and for waterproofing. Available in many materials for different skin sensitivities.
Adhesive remover
Helpful for removing wafers/tape and cleaning residue.
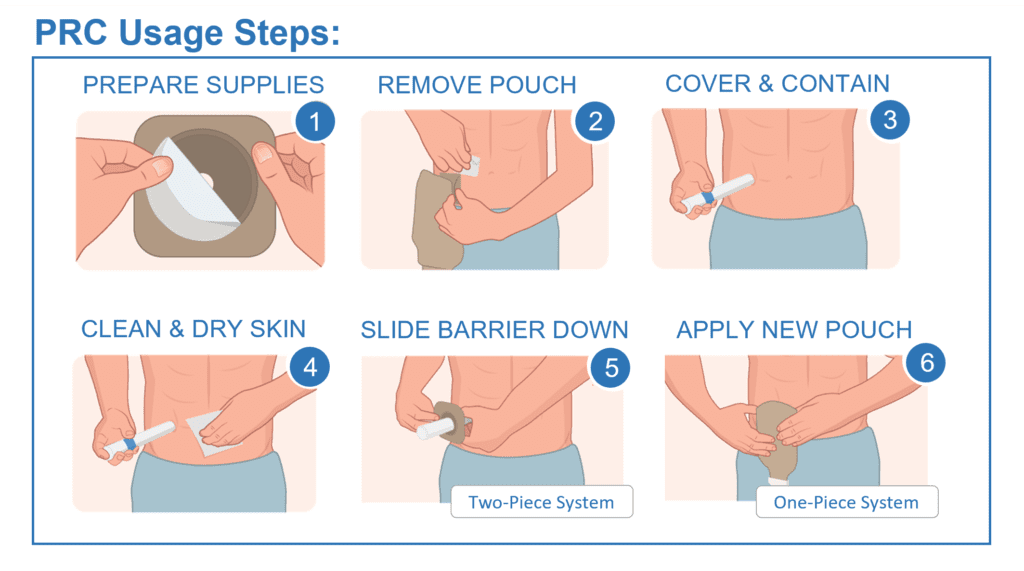
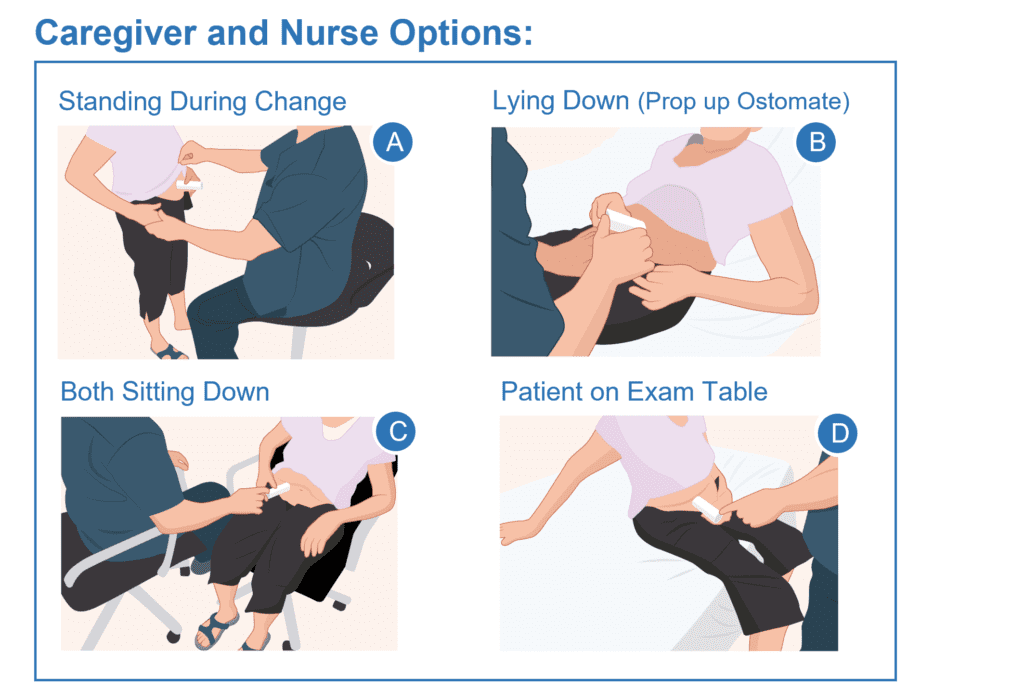
Pouch Replacement Cartridge (PRC)
A single-use cartridge that can temporarily cover the stoma during pouch changes to help contain output, reduce effluent contact with skin, and allow time to clean and dry peristomal skin.

Expert Review and Collaboration:
Maky Suarez, MSN, RN, WON, COCN –Mary Lou Boyer, BS Ed, RN, WOC Nurse
Joy Hooper, RN, BSN, CWOCN, OMS, WCC, WCEI®Clinical Instructor –Anita Prinz, RN, MSN, CWOCN Debi Fox, Ostomate, Ostomy Education Consultant –Reed Johnson, Editor,Illustrations, Graphic Design
FAQ: Types of Ostomy Pouching Systems
What’s the difference between a one-piece and two-piece ostomy system?
A one-piece system combines the skin barrier/wafer and pouch into a single unit. It’s simple, but when you change the pouch, you change the whole thing (including the barrier).
A two-piece system has a separate barrier/wafer that stays on your skin and a pouch that attaches to it. The big advantage is you can change the pouch without removing the barrier every time.
What does “drainable” vs “closed-end” mean?
For colostomy and ileostomy pouches:
- Drainable (open-ended): You empty it while it’s still attached to your body. It usually requires a closure device (traditionally a clamp/clip).
Closed-end: Sealed at the bottom and typically discarded after one use. UOAA notes these are most commonly used by colostomates who can irrigate or who have regular elimination patterns.
What is a flange in ostomy supplies?
In UOAA’s wording, the barrier/wafer is part of a “flange” unit in a two-piece system. The pouch has a connecting ring that attaches mechanically to the flange (often a snap-ring style connection).
What does a convex barrier do?
A convex skin barrier is curved (not flat) and is designed to press inward on the skin next to the stoma. UOAA explains that convexity can provide a gentle push that helps the stoma protrude outward, which can help output go into the pouch instead of sneaking under the barrier (aka leaks).
When should I talk to an ostomy nurse about leaks or skin irritation?
UOAA is very direct here: contact your stoma/ostomy care nurse if you have skin irritation or recurrent leaks under your pouching system or skin barrier (plus several other symptoms they list).
Also, on the pouching systems page, UOAA specifically says that if you’re having trouble with your current system, you should discuss the problem with an ostomy nurse or other caregiver and that it’s common to try several types until you find what works best.
Contact Us

United Ostomy Associations of America
P.O. Box 2293
Biddeford, ME 04005-2293
Call us toll-free at: 1-800-826-0826.
Our Information Line hours are Monday-Friday, 9am to 3pm EST. If you have an emergency, please dial 911 or contact your local medical professional.
Please understand that UOAA is a private, nonprofit, advocacy and informational organization. We are not a medical facility and we do not have medical or legal professionals on staff. Therefore, UOAA does not provide Medical, Mental Health, Insurance or Legal Advice. Visit UOAA Virtual Ostomy Clinic provided by The Wound Company for non-emergency, virtual ostomy support.
Get Involved
UOAA is the leading organization proactively advocating on behalf of the ostomy community. Recognizing that we are always stronger together, we encourage everyone to get involved by joining our Advocacy Network. We’ve also created several Advocacy Tools and Resources to help you successfully advocate on behalf of the ostomy community to ensure every ostomate receives quality care.