My name is Katie Lee, and I was diagnosed with stage 1 rectal cancer at age 33, only eight months after the birth of my second child. My tumor was […]
In celebration of Wound, Ostomy, and Continence (WOC) Nurse Week 2021, help us to shine a bright light on these special nurses. They give us the hope, support, and specialized care needed to thrive in life with an ostomy.
WOC nurse volunteers spend countless hours advocating, leading support groups, educating, fundraising, and supporting UOAA programs and services. UOAA recognizes that not all ostomy patients have access to a WOC nurse and we’ll continue to advocate for access to a specialized ostomy nurse from preoperatively when your stoma site is marked through an ongoing lifetime continuum of care as outlined in our Ostomy and Continent Diversion Patient Bill of Rights.
We asked UOAA’s social media community to share how a WOC nurse has made a difference in your life, health, or support group. We hope more nurses will consider this rewarding specialty. Thank you WOC nurses, you are our guiding lights.
I would like to thank my WOC nurses who have and continue to support me as an ostomate. My nurses inspired me so much I went to nursing school and graduate this month with a BSN and plan on continuing on. To become a WOC nurse myself! Thank you WOC nurses! -Katie Lee
“My WOC was a lady named Gayle. She helped my Mom so much with me. I remember many visits to the ER ward and having her there. She was funny, nice and on it. I used to love seeing her. She stayed by my side from 3-6yr old into my adulthood. She fought hard to find a bag that was the perfect fit for me. She got a new product in and it changed my life significantly, she fought tooth and nail to keep me in that bag, even when Canada decided to stop offering it openly. I still wear that brand to this day. I always heard rumors she was also an Ostomate and I can’t say how long. That made me love her more. I will never forget those who had a hand in my welfare and saw me through their entire career. I miss her and the others immensely. Jody is my new WOC and although I rarely need her, she’s there to help, even if it’s a panic situation that couldn’t wait for an appointment.” –Camille C.
“Joanna Burgess Happy WOC Nurse week. You have been a true Angel of Mercy for me over the years!” –Col Justin Blum
“My son’s WOC nurses at CHLA were awesome!!” – Teri C.
I am a WOCN and worked with MANY ostomy patients in the past. The thanks go both ways — I have never (in a long nursing career) felt as appreciated for my clinical skills and assistance as I do when working with people with an ostomy. They are the reason I have stayed in nursing. -Cris R.

This is Karen with my husband at his 55th birthday party in 2019 -Pam Allen Williamson
We have 3 great WOC nurses in our community that come to our ostomy support meetings Karen Eubank, Michael Byars and Jason Pratt. Michael went above and beyond by creating a weekly outpatient ostomy clinic after I told him I learned some cities had those while attending a UOAA conference. Karen who has been coming to our meetings for over a decade, hosts many of our support group parties at her house, works at the ostomy clinic on a regular basis, pays to store donated supplies and often helps people after hours. Both of them visit my husband when he is hospitalized, came to the house to visit him when he was home on hospice and came to his funeral. We are extra grateful to Karen because before he left the hospital on hospice she applied a special high output bag connected to bed drainage bag to minimize the family’s need to interact with the ostomy. Karen who is a neighbor told me that she would come change the bag twice a week. The hospice nurse was fascinated and stayed late to watch Karen change it out. He was going to stay in the hospital as long as they would let him to avoid family having to deal with his bag because he had always been so independent with it until nearly the end. Karen’s solution allowed him to come home and be surrounded by family caregivers that loved him and have wonderful conversations remembering fun times and having important conversations instead of the visitor limitations hospitals right now. We are so grateful to her for this and hope it will benefit other families of bed-bound patients. BTW we still fondly remember my husband’s first WOCN Nurse Licklighter who was a nurse at Keesler AFB in 1993. She marked him before surgery and taught him how to handle his bag and he kept her handwritten instructions forever and sometimes copied them for others. -Pam A.W.
I can’t thank the nurses at Ohio Health Riverside Hospital they helped me so much and made an otherwise difficult transition quite non traumatic! –Carol B.
Thank you to Erin and Vanessa at New York Presbyterian! –Jameson Cycz
The ConvaTec nurse Lorelei. She has been a stoma saver. She helped me troubleshoot my leaking problem, got me into a new pouching system, that is awesome and when I ran out of samples and am in limbo with my supply company in getting the new pouches and other supplies, she set me up with a holdover supply, so that my stoma won’t be continuously injured by my current pouches.- Susan Gentner
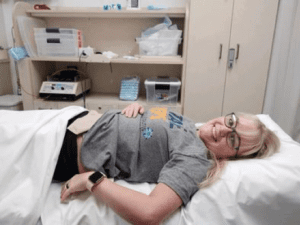 I’m thankful for all of the WOCNs I have been to. Some I’ve known for many years. They are very knowledgeable and helpful with various products.I also want to give a shoutout to our great WOCNs at 11 Health & Technologies for being amazing for our team and patients. ? –Megan Alloway
I’m thankful for all of the WOCNs I have been to. Some I’ve known for many years. They are very knowledgeable and helpful with various products.I also want to give a shoutout to our great WOCNs at 11 Health & Technologies for being amazing for our team and patients. ? –Megan Alloway
Amazing Aimee Frisch. The best WOCN in know. Love you. -John Pederson
Happy #WOCNurseWeek2021! What you do for ostomy patients and the impact you make is immeasurable! Plus we are grateful for all that you do to support UOAA and our advocacy program! You are advocates for patients and can influence change. Shine on! @UOAA_Advocate -Jeanine Gleba
 I want to tell my story concerning my ileostomy in order for people to understand how it is living with one and how a person can live a normal life and more.
I want to tell my story concerning my ileostomy in order for people to understand how it is living with one and how a person can live a normal life and more.
I had my original ostomy surgery 49 years ago in 1972 – you can imagine how surgeries, techniques and medicines have progressed since then. Twenty-five years old at the time, I spent several weeks in the hospital recovering. At age 24, I experienced my most serious bout of ulcerative colitis, and after several months with a tremendous amount of blood loss, it was determined that I would be better off having my colon removed, living with an ileostomy and staying alive, period.
Needless to say, it was a difficult transition from a “normal” body to one with a bag/pouch attached to my abdomen forever. Discharged from the Navy a couple of years before my surgery, I had been enrolled at the Ohio State University, and so decided to finish school and get my teaching degree. After the original colectomy procedure, a few more surgeries were required to correct a protruding ileum, but finally things settled down to where I could get back to a normal life.
Trying to live life to the fullest, I appreciate every day that I’m alive.
Admittedly, life was a little rough for a couple of years after my surgery, especially when it came to dating. I was embarrassed to mention my ileostomy and even today, am reluctant to tell people. it’s probably a personality trait, but I feel I need to get to know people before I tell them about me. However, the day I met my wife-to-be, I told her about my ileostomy and we have been together ever since; go figure.
In the past 49 years, I have graduated from college, gotten married, had a son, worked for the government, taught high school, coached football and tennis, and traveled extensively. I played tennis for many years, as well as golf. I’ve camped in the Rockies, the Grand Canyon and the Grand Tetons, traveled throughout the United States, hiked the Camino di Santiago in Spain and spent many vacations in Italy. I’ve hiked parts of the Appalachian trail and still love hiking to this day. An avid speed walker for the last 10 years, I qualified for the Senior Olympics two years ago and this year.

Working as a personal trainer for 15 years has been a satisfying retirement job. I still play golf and walk four to five miles almost every day. I wrote an exercise manual a few years ago, The Hotel Motel Workout, and have filmed and posted exercise videos on the internet.
Trying to live life to the fullest, I appreciate every day that I’m alive. One further surgery was necessary for a revision to my ileostomy a few years ago, but I feel blessed that the doctors talked me into having the original ostomy surgery 49 years ago. Life is good.
When Paige started seventh grade, she was excited to meet new friends and begin new classes, like most 12-year olds! Her life quickly changed when she began to experience medical complications. At the beginning of seventh grade, Paige started having to make frequent visits to the bathroom, as much as 12 times a day. Paige and her family sought out answers and treatment at a nearby hospital where the doctors found a parasite in her colon called cryptosporidium, which causes diarrheal disease.
Due to her Ulcerative Colitis diagnosis at the age of 10, the parasite was life-changing for Paige, as it destroyed her colon. “They told me that with how bad my colon was, I should have died.”
Paige went through a variety of treatments to save her colon. This started with receiving Remicade as an IV treatment…Paige’s body did not respond well. The next step in treatment was to try a j-pouch, again her body did not respond well to this treatment, but a j-pouch was tried one more time with the same outcome. After her two failed j-pouch operations, Paige continued to be sick and only had 8 feet of intestines left. Her mother, Cristy, discussed with her doctors to do something different since the j-pouch was not working, and that’s when Paige had surgery to receive a permanent ileostomy. After months of hospital stays, her life was saved with her ostomy. Paige’s journey doesn’t stop there. After being discharged from the hospital, Paige had trouble finding a pouching system that helped provide a secure fit to her body.
“We left the hospital with an ostomy pouching system that had a 12-hour wear time, at best,” says Cristy. “I went mama mode and searched for a better product. Luckily, we found a great gal on the other end of the Coloplast® Care phone line who answered all our questions and gave us just that!,” she said.
Once Paige found a pouching system that worked for her and started to gain her confidence back, she saw the need to create more resources for teenagers living with an ostomy, because there wasn’t much out there!
“I play volleyball, I go to camps that are just like me (Youth Rally), I attend high school dances, I go on dates…I do it all! Coloplast helped me find the best fit for my body. They may be able to help you too. I have used Coloplast for 4 years now and I still feel confident in my pouch.”
According to Paige, living with her ostomy is not always easy. Along with the physical challenges, there are mental challenges from her experiences as well. Paige encourages anyone experiencing mental challenges to speak up and find someone to talk with.
To help other teenagers living with an ostomy, Paige and Cristy contacted Coloplast, and they partnered together to create a care guide specifically for teenagers!

Throughout this booklet, Paige hopes to share the tips and tricks that worked for her as well and provide answers to common questions.
Download a free copy of this teen resource here: https://www.coloplast.us/landing-pages/teen-booklet/
*Paige is a Coloplast product user who has received compensation from Coloplast to provide this information. Each person’s situation is unique, so your experience may not be the same. Talk to your healthcare provider about whether this product is right for you.
Editor’s note: This article is from one of our digital sponsors, Coloplast. Sponsor support along with donations from readers like you help to maintain our website and the free trusted resources of UOAA, a 501(c)(3) nonprofit organization.
Michael Seres started 11 Health as a direct result of his experiences as an ostomate. He had suffered with Crohn’s disease for over 30 years and after a small bowel transplant, he needed an ostomy. He felt alone and powerless. The bags were hard for him to get used to and they did not help to manage his condition – they just collected output. He started blogging and tweeting about his journey and found tens of thousands of patients who felt the same way but were too anxious or disempowered to do anything about it. Michael made a commitment that he would devote his life to making a difference for these patients.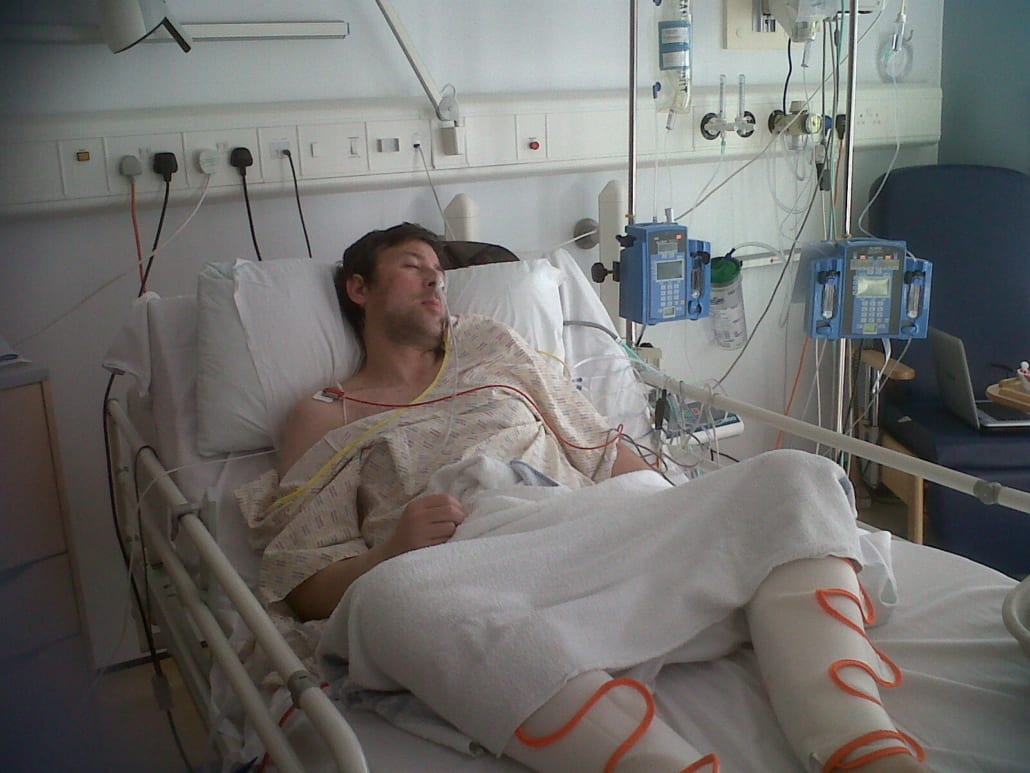
Despite his health struggles, which included fighting and beating cancer multiple times, he found the strength to start a healthcare company that shares his single-minded focus of helping patients, and in particular ostomates. The company is called 11 Health as Michael was the 11th person in the UK to have had the pioneering transplant procedure. Only a few of the 10 that went before him survived the procedure. Michael did not just survive, he thrived and accomplished so much in his short life.
Advocacy was always a part of Michael’s life. He always found time to prioritize it amidst the challenges of running an international business and managing his health. In his talk at Stanford Medicine X in 2017, he talked about a revolutionary idea of using social media for doctor-patient communications. Michael believed that patients were the most underutilized resource in healthcare and he spoke beautifully about it in his famous TEDx Talk in 2018. The need for the patient to be at the center of patient care ran through his core. He felt that patients should not be passive end users. Instead, patients should be engaged in medical decision making and empowered by education and self-care tools. Michael’s reach was spread wide and he advocated for patients to the leadership of Google and even on a panel alongside Bill Clinton.
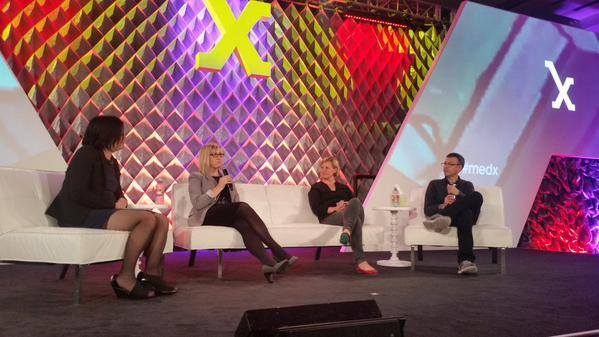
We lost Michael last year. Whilst our hearts are still filled with sadness, we are more determined than ever to deliver his vision of changing healthcare and making it patient centric. He believed passionately in the ‘everyone included’ philosophy. A movement for change supported by doctors, nurses, policy makers but most importantly, patients. Making that change will be Michael’s legacy.
We are creating a special birthday Gutsy Gathering on March 23 from 3-7pm EST in Michael’s memory. It will not be a day to mourn. It will be a day to celebrate the achievements of an extraordinary man by inviting some equally extraordinary people to talk about their personal or professional involvement in the patient experience. Sessions will focus on themes relating to advocacy, confidence, community, and change.
The Michael Seres birthday Gutsy Gathering will be an annual event and an opportunity for friends to meet in a face-to-face setting. This year it will be virtual, with speakers joining us from around the world from across the ‘everyone included’ spectrum. The live sessions will run from 3-7pm EST and participants can come and go as their schedules allow. The event is free, and registration is required at www.gutsygathering.com. Our esteemed list of speakers continues to grow and can be found on the registration page. Please join us!
Editor’s note: This article is from one of our digital sponsors, 11 Health. Sponsor support along with donations from readers like you help to maintain our website and the free trusted resources of UOAA, a 501(c)(3) nonprofit organization.
Colorectal cancer survivor Allison shares her ostomy story. “No one truly understands what you are going through physically and psychologically more than those who have been there themselves.” Check out her mythbusting videos and more.
Embracing Ostomy Advocacy and Giving Back
By Angie Davenport
I’ve had my ileostomy for 38 years due to ulcerative colitis but I only recently went public to encourage other ostomates. Over the years I’ve helped many individuals by word of mouth while keeping my ileostomy private to the outside world. I have always wanted to be a blessing on a wider scope though to others with ostomies.
I was first diagnosed with ulcerative colitis in 1980 when I was three months pregnant. At first, I thought it was pregnancy symptoms. After a major episode, I was treated with medication for ulcerative colitis. My son, James was born a few weeks early due to complications.
After the birth of my son in March of 1981, everything was under control and I eventually relocated from Warren, Ohio to Atlanta, Georgia. While living in Atlanta I had a major setback with ulcerative colitis and I had to fly back to Ohio immediately and went directly to the hospital.
After several weeks of treatments in the hospital, my doctor came into my hospital room one night and said we have to do surgery or you won’t make it 24 hours. I’ll never forget my mom crying and praying for God to give her my disease so I could have a normal life.
When I received my permanent ileostomy in March of 1982 I was a young 23-year-old single mom. It was the day before my son’s first birthday. I had never heard of an ostomy. When I woke up in ICU I was devastated, ashamed and frightened. I thought my life was over.
Once I became strong enough physically and mentally I moved back to Atlanta. I was still feeling ashamed and frustrated until my physician in Georgia recommended I attend the local United Ostomy Association (the precursor to UOAA) support group.
While living in Atlanta I became very involved with the UOA group and completed the visitor training program. I enjoyed visiting new ostomates at the hospital. I felt the freedom to be involved because no one really knew me in Atlanta. I remained active until I relocated back to Ohio in 1985. That same year I married my high school sweetheart and we will celebrate 36 years of marriage in November.
Although I was very private about my ostomy I was very successful in my career. I became the first African American female officer at our local bank and functioned in several positions without the exposure of my ileostomy. After the downsizing of my employer, I later worked 10 years at Great Lake Cheese until retiring in 2016.
What is my purpose in life? How can I make my mom proud?
I’ve enjoyed my life as an ostomate. I love traveling, cruising and shopping. I was known in the business community as a person that loved to dress. I taught Dress for Success at the bank for all new tellers.
 The past few years were filled with so much grief, with the most current being the death of my mom on July 4th 2019, only three days after my 60th birthday. I was feeling the deep void of losing a brother and both parents within 4 years, depression was setting in. I had support but I felt helpless and lost. What is my purpose in life? How can I make my mom proud?
The past few years were filled with so much grief, with the most current being the death of my mom on July 4th 2019, only three days after my 60th birthday. I was feeling the deep void of losing a brother and both parents within 4 years, depression was setting in. I had support but I felt helpless and lost. What is my purpose in life? How can I make my mom proud?
Most will remember 2020 as a horrific year with so much sickness, death and devastation from a deadly pandemic. For me, I utilized the time to seriously seek God for a purpose in my life and being quarantined turned out to be a blessing in helping me find my purpose.
I knew my testimony would bring awareness and hope to so many people.
I became more involved via social media with other ostomates. I’ve met some wonderful friends and it became rewarding to encourage others that had shared similar experiences as me. My heart was really saddened when I read an article about a young man that had gone to court for the right to die because he didn’t want to live with an ostomy. I wept. Also seeing how some individuals can’t afford the basic ostomy supplies and had to use grocery store bags and tape to secure their ostomy bags was heartbreaking. I knew then, that there was so much more I could do for the ostomy community. I knew my testimony would bring awareness and hope to so many people.
As a member of Jearlean Taylor’s Ostomy Stylzz Facebook Group I participated in a virtual fashion show. She is a personal inspiration to me and that show boosted my confidence to a much greater level. I felt a relief to go public. I chose August 14th, 2020 to go live on Facebook and share my story. I felt such freedom once I finished. There were family members, coworkers, church and community friends that responded and supported me in disbelief. For the past 38 years, they never knew I had an ostomy.
One family friend messaged me and told me that he was scheduled for surgery but has canceled many times, but because of my video he felt he could now go through it. I still check on him to make sure he’s not having any problems. That made going public all worth it. But what else could I do?
I decided to participate in the Run for Resilience Ostomy 5K. I registered over 20 walkers to participate virtually in several cities and I exceeded my fundraising goal by almost 100%. The highlight of the day was my local mayor stopping by to present me with a proclamation from the City of Warren in support of ostomy awareness. Our local newspaper also highlighted the event.
…because of my video he felt he could now go through it.
After posting my Ostomy Awareness Day photos and story on Facebook I was contacted by so many family and friends willing to support me in the future.
With the pandemic still active, I’ve been limited in getting out in the public but I do try to make an effort to encourage other ostomates daily. I’ve connected with my local Affiliated Support Group leader and I’m looking forward to greater things once we can meet publicly.
On, March 6, 2021 I will be a 39-year ostomate.
I’m on Facebook and I have a Youtube video discussing my ostomy journey.
I’m free, living with my ostomy!
Discovering Strength in the Struggle from J-Pouch to a Permanent Ostomy

If you asked me 20 years ago when I was in college if I thought I could be a strong ostomate, I would have just stared at you in shock. Strength and I were not the best of friends. In fact, it was one of the things I often questioned about myself. I had no idea what was something worth crying about.
That all changed three years ago when I was put to the test when I went from sudden rectal bleeding as a result of ulcerative colitis, to having to remove my colon in a matter of four months. During the next three years, I had four more operations from trying the j-pouch and failing, to finally getting a permanent ostomy just this past December.
Somewhere along the way, I found my strength. I dealt with major emotional and physical changes faster than I could even process. I had to adapt to a whole new way of life and a whole new way of looking at myself.
Somewhere along the way, I found my strength.
These three years have been incredibly hard. They have tested me in every way, broken me down to smithereens of myself, and caused me to question everything. The true strength that just suddenly overcomes you when you least expect it is something you don’t really understand until you are there and have no other choice. Life after that is forever changed.
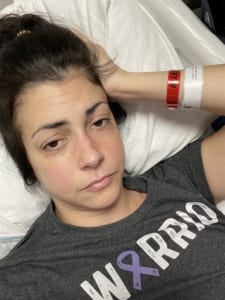 Along the way, I started to feel strong. I was amazed by what both my body and my mind could accept and turn into a positive. I started to really take care of my physical health, and in the three years that I have been the sickest in my life, I became the most physically strong I have ever been by participating religiously in barre class. This physical strength, along with the help of the ostomy community, is what helped me to then discover my mental strength.
Along the way, I started to feel strong. I was amazed by what both my body and my mind could accept and turn into a positive. I started to really take care of my physical health, and in the three years that I have been the sickest in my life, I became the most physically strong I have ever been by participating religiously in barre class. This physical strength, along with the help of the ostomy community, is what helped me to then discover my mental strength.
I literally stared death in the eye and won. It is hard to even write that today.
Feeling very alone, I stumbled across some ostomy bloggers one night while scouring the internet. Reading their patient stories blew my mind at the time, because I didn’t comprehend how they could just accept living with an ostomy. But all that changed and I began to understand when I was so sick that it was no longer a choice if I wanted to keep being a mommy. The decision to have a permanent ileostomy was the best choice I ever made.
This physical strength, along with the help of the ostomy community, is what helped me to then discover my mental strength.

I just had what I hope to be my final surgery and got my permanent ostomy on December 1, 2020. Since then, I have made some promises to myself. I want to be my absolute best version of myself now that I am able to really live again. I want to help as many people with IBD and facing the possibility of an ostomy as I can. I want them to see what I have come to see, that they too can use such an incredibly difficult period in their life to find their strength and their best version of themselves.
“God said to me, I am going to show you pain. And then you are going to help other people who are in pain because you understand it” (Lady Gaga).
Outdoor Adventure Does Not Stop with an Ostomy and IBD.
Hi my name’s Charlotte!
I grew up in New Hampshire as the youngest of three sisters. I had a pretty normal childhood and was raised by a wonderfully supportive family who fostered in me a sense of independence and love of adventure. In 2007, at the age of 17, I was diagnosed with ulcerative colitis. That diagnosis later changed to Crohn’s disease, and it changed my life forever.

My IBD progressed rather quickly and about nine months after my original diagnosis, I had my colon removed, a temporary ostomy, and a j-pouch created. I lived with my j-pouch for five years, and those were some of the toughest years of my life. Despite a failing jpouch, pooping my pants every day, and a variety of other debilitating symptoms, I was determined to continue living my life. I was able to graduate from high school, bike across the country while in college, and complete my academic coursework as an Occupational Therapy student on time (despite dropping out of college in my Sophomore year because of my Crohn’s disease). I was not going to let Crohn’s get in my way.
 In 2013 after agonizing over the thought of ostomy surgery (I had been adamant for years that I would not have an ostomy), I finally told my surgeon I was ready, and underwent surgery for a permanent ileostomy. I felt prepared for ostomy surgery this time around because I went to local support groups in Boston to learn more about living life with an ostomy. I also found a surgeon who understood me and what I wanted out of life. My ostomy changed my life again, and this time for the better. I’ve had 3 stoma revisions and my Crohn’s does pop up every now and then, but I have so much more freedom in my life with my ostomy.
In 2013 after agonizing over the thought of ostomy surgery (I had been adamant for years that I would not have an ostomy), I finally told my surgeon I was ready, and underwent surgery for a permanent ileostomy. I felt prepared for ostomy surgery this time around because I went to local support groups in Boston to learn more about living life with an ostomy. I also found a surgeon who understood me and what I wanted out of life. My ostomy changed my life again, and this time for the better. I’ve had 3 stoma revisions and my Crohn’s does pop up every now and then, but I have so much more freedom in my life with my ostomy.
In 2014, after graduating with my Master’s in Occupational Therapy, I was able to move to Alaska to take my life back and pursue a life of outdoor adventure (and work). I started sharing more about my ostomy with my community which increased my confidence. I worked to establish a collaborative medical team, including my surgeon, GI doc, and physical therapist/pelvic floor therapist who have helped me take control over my life and continue an active lifestyle. I’m a passionate OT working in Anchorage. I enjoy running, biking, skiing, climbing, hiking, backpacking, camping, and spending any time outdoors. My family, boyfriend, and friends are my greatest sources of support, and they inspire me to live my life fully.
In addition to my passion for the outdoors and exercise, I enjoy empowering others to learn more about themselves and how to thrive with an ostomy. When I first had my ostomy, there weren’t many resources out there, but I stumbled upon the Ostomy Outdoors blog which provided helpful resources for my outdoor journey with my ostomy. That’s in part why I blog to support other ostomates returning to active lifestyles after ostomy surgery. And I recently started my business, Restorative Ostomy Solutions to empower Occupational and Physical Therapists to feel more confident working with ostomy patients.
Through rehabing myself from six major abdominal surgeries, I have learned what it takes to pick myself up after each setback and continue on my life journey. Because life if so much more than my diagnosis and my ostomy!
A research study about the benefits of perioperative self-management support for ostomates
Ostomates are not only dealing with intestinal concerns but are also at risk for a multitude of complications. Data shows that 38% of ostomy patients find themselves back in the emergency room or  being admitted within the first 90 days post operatively [1]. This is one of the highest rates of readmission when compared to other types of surgery. The most common cause for re-admission is dehydration, at approximately 40% of post ileostomy readmissions [2]. We also know that 84% of ostomy patients develop skin issues. The causes of these can be chemical, mechanical, or microbial, and possibly avoidable. Ostomates also have significantly increased healthcare costs, especially when affected by peristomal skin complications, and leakage [2]. It is known that 25% of ostomates develop renal failure within two years. The complications these patients encounter require 7x more outpatient visits than the average patient. And 29.1% of ostomates experience readmission which costs approximately $16,000 per patient [1]. These statistics show that specialized care for these patients is imperative to improving patient outcomes in this patient population.
being admitted within the first 90 days post operatively [1]. This is one of the highest rates of readmission when compared to other types of surgery. The most common cause for re-admission is dehydration, at approximately 40% of post ileostomy readmissions [2]. We also know that 84% of ostomy patients develop skin issues. The causes of these can be chemical, mechanical, or microbial, and possibly avoidable. Ostomates also have significantly increased healthcare costs, especially when affected by peristomal skin complications, and leakage [2]. It is known that 25% of ostomates develop renal failure within two years. The complications these patients encounter require 7x more outpatient visits than the average patient. And 29.1% of ostomates experience readmission which costs approximately $16,000 per patient [1]. These statistics show that specialized care for these patients is imperative to improving patient outcomes in this patient population.
A recent study published by the American Society of Colon and Rectal Surgeons shows how one company, 11 Health and Technologies, is utilizing a novel care approach to improve the quality of life and outcomes in this type of patient. The company developed alfred: SmartCare, a unique care model designed to meet the specialized need of ostomates. The program consists of a SmartBag and SmartWafer, mobile application, patient coaches (who were/are also ostomates, trained to support this type of patient) and the nursing team. The patient wears the SmartBag and SmartWafer, which submits data to the mobile application and clinical dashboard. The data is visible to the patient, their coach, the nursing team and the patient’s clinicians to be used to identify trends and abnormalities in the values. The patient can see how much output they have expressed and what the temperature is of their peristomal skin. These data points can help to curtail oncoming hydration issues or infections. When abnormalities are identified, the coach can work with the patient to provide education and can escalate issues to the nursing team for medical guidance.
In the study, the outcomes of 66 new ostomates from 19 different states were monitored for the first 30 post-operative days. The study showed that close monitoring of ostomy output volume as well as perioperative self-management support can significantly reduce the rate of hospital readmissions in the first 30 days after ostomy surgery.
Patients and healthcare providers should be open to the use of innovative programs that use remote monitoring along with telehealth, as they can be beneficial in improving the outcomes of patients in the immediate post-operative period.
To read the full study, visit the Diseases of the Colon & Rectum online at: https://journals.lww.com/dcrjournal/Citation/2020/12000/Improved_30_Day_Surgical_Outcomes_in_Ostomates.17.aspx
Editor’s note: This article is from one of our digital sponsors, 11 Health and Technologies. Sponsor support along with donations from readers like you help to maintain our website and the free trusted resources of UOAA, a 501(c)(3) nonprofit organization.
[1] Tyler, J. A., Fox, J.P., Dharmarajan, S., Silviera, M. L., Hunt, S. R., Wise, P. E., Mutch, M. G. (2014). Acute health care resource utilization for ileostomy patients is higher than expected. Diseases of the Colon & Rectum, 57(12), 1412-1420.
[2] Justiniano, C. F., Temple, L. K., Swanger, A. A., Xu, Z., Speranza, J. R., Cellini, C., Salloum, R. M., & Fleming, F. J. (2018). Readmissions With Dehydration After Ileostomy Creation: Rethinking Risk Factors. Diseases of the colon and rectum, 61(11), 1297–1305. https://doi.org/10.1097/DCR.0000000000001137
[3] Taneja, C., Netsch, D., Rolstad, B. S., Inglese, G., Eaves, D., Oster, G (2019). Risk and economic burden of peristomal skin complaints following ostomy surgery. Journal of Wound, Ostomy and Continence Nursing, 46(2), 143-149.
[4] Fearn, Robert I. M.D., M.R.C.P.1,2; Gorgun, Emre M.D.3; Sapci, Ipek M.D.3; Mehta, Saahil N. M.D.2; Dinh, Binh B.S.2; Yowell, Quinn V. M.S.2; Eisenstein, Samuel M.D.4 (2020). Improved 30-Day Surgical Outcomes in Ostomates Using a Remote Monitoring and Care Management Program: An Observational Study. Diseases of the Colon & Rectum: December 2020 – Volume 63 – Issue 12 – p e581-e586.
Excerpt from the story One Man’s Journey From Bladder Cancer
 The day for my fourth cystoscopy had finally arrived. My doctor smiled and asked if I was ready for this exam. With a nod from me, turned off the lights, and guided the instrument into my body. He reiterated that there were cells in my bladder. I felt a large lump in my throat, and my face began to flush. Because these cells had been so aggressive and returned after the three previous treatments, there were no additional medications that could be used. He explained there were several other choices: (1) do nothing, (2) having a neo-bladder constructed, and (3) urostomy surgery. We would discuss these options in a few weeks.
The day for my fourth cystoscopy had finally arrived. My doctor smiled and asked if I was ready for this exam. With a nod from me, turned off the lights, and guided the instrument into my body. He reiterated that there were cells in my bladder. I felt a large lump in my throat, and my face began to flush. Because these cells had been so aggressive and returned after the three previous treatments, there were no additional medications that could be used. He explained there were several other choices: (1) do nothing, (2) having a neo-bladder constructed, and (3) urostomy surgery. We would discuss these options in a few weeks.
Note: Each person is unique, and so are the methods used to treat this cancer.
An appointment was made for this consultation, and within two weeks I would see my doctor. In the interim, I had given careful thought to all three options. Doing nothing could be taking a huge risk. If the cells should travel into the muscles of the bladder, my life would definitely be in jeopardy. There was a chance these cells might metastasize to other organs of my body. We could wait and see if they did travel. However, this was not a chance I wanted to take. A neo-bladder, created from my intestines, would allow me to still urinate through my penis, but required much effort to adjust to, and a longer recovery time. It also brought with it the possibility of incontinence, or not working properly, necessitating additional surgery. The neo-bladder is also a relatively new form of treatment that many urologists choose not to use.
My final option was to have my bladder and prostate gland removed surgically. Compared to the construction of a neo-bladder, the recovery time was shorter. It had been proven to be successful in eliminating cancer and allowing patients to resume normal lives. This return to normalcy would occur after an initial adjustment period when the patient learns how to use and care for the Ostomy Pouch. Over time this would become routine.
After more consultation… My faith and confidence in my physician and in my decision to receive “external plumbing” (the ostomy pouch), gave me peace of mind up to the day of surgery.
Road to Recovery
My hospitalization would soon be terminating. However, before leaving I insisted on seeing the Ostomy Clinical Nurse Specialist (CNS) making sure that I felt confident applying and removing my ostomy pouch. Even though the hospital wanted to discharge me, I was persistent. Managing my ostomy pouch will be a lifelong endeavor. The CNS reviewed the process of changing the pouch and demonstrated it several times. Her patience, warm smile and reassurance made me feel capable of handling this task on my own and confident to be discharged from the hospital. (Keep in mind that it is a patient’s right to determine whether or not he/she is ready to leave the hospital)
On My Own
After then spending time in a rehabilitation facility It was great to finally be home, and feel independent. As a widower, I was fortunate enough to have met a woman whose companionship helped to avoid a great deal of loneliness. Had she not been there, returning to my empty house would have heightened my feeling of isolation. Thinking back, yes, I certainly could have managed by myself. However, her presence made my transition from the hospital, rehabilitation facility, to home that much easier. Many patients who are single, or don’t have family/friends to support them when returning home, can find this a mixed blessing. They may feel independent, yet experience loneliness. Anxiety may occur over fear they may lack the ability to manage by themselves. The services of a visiting nurse, physical/occupational therapist, or a mental health professional can be provided to alleviate these concerns. The availability of these services were discussed during my exit conference from the rehabilitation center.
Adjustments To Be Made
Anxiety arose as I continued on my journey to recovery. The first of these emotional hurdles, especially for newbies is attaching an ostomy bag securely, preventing leakage. Having a spare pouch and supplies, along with a change of clothes, solves this concern. My medical supplier provided a small pouch to carry these items. Initially, I had many questions about the ostomy pouch. However, when various concerns arose, (getting this device on properly, leaks, or supplies), my nurse responded to these questions promptly and gave me the reassurance I needed. Trust me, I continued to have questions for months after my surgery. By that time I built up enough confidence in using this device, and it became more routine. Ostomy nurses serve as a great resource. They also recommended a monthly support group. Knowing what others have gone through, and how they dealt with their post-surgical life, can be very helpful.
pouch and supplies, along with a change of clothes, solves this concern. My medical supplier provided a small pouch to carry these items. Initially, I had many questions about the ostomy pouch. However, when various concerns arose, (getting this device on properly, leaks, or supplies), my nurse responded to these questions promptly and gave me the reassurance I needed. Trust me, I continued to have questions for months after my surgery. By that time I built up enough confidence in using this device, and it became more routine. Ostomy nurses serve as a great resource. They also recommended a monthly support group. Knowing what others have gone through, and how they dealt with their post-surgical life, can be very helpful.
Thanks to my Ostomy Clinical Nurse Specialist (CNS), two additional Leak Prevention Supplies (LPS) were suggested: (1) A belt attaching to both sides of the bag to hold the wafer and pouch more securely in place, and (2) A U-shaped elastic barrier fitting around the bottom of the adhesive which attaches to your body and wafer. These items can be requested from your medical supplier, and may help give some peace of mind. These remedies have worked for me. Timing for emptying the pouch is another adjustment. This usually occurs when the bag is 1/3 to 1/2 full. For me, this point is reached hourly, possibly because my kidneys are located in the front of my body. For others, this may occur up to 2 1/2 hours. However, empty points are individualized.
Timing this process initially limited me from going places beyond one hour. For many of us, noting the location of bathrooms is something we typically make prior to leaving for a destination. Even before surgery, I spotted the location of the bathrooms. If you think about it, for many people who still have their bladder, nature calls them frequently. Whenever this need arises, they go on “bathroom alert.” We don’t have this urgency or stress of finding a bathroom as they do. We can anticipate when to empty our pouch and can plan our pit stops in advance. This is a positive of having an ostomy pouch. Think about that.
Ways to judge the timing of emptying the pouch also become routine. Checking your watch, cell phone, or clock helps the timing factor. Generally, If I were to go to a restaurant, at most, twenty minutes away from home, I’m able to wait until I have eaten my meal before emptying my bag. For others, gauging the timing may involve the length of events (movies, shows, etc.) or the time it takes to reach a destination. It’s an awareness that you will develop. During your recovery period, fatigue could be an issue. Initially, I tried to do too much, too soon. Don’t fight this feeling. You don’t have to prove anything to yourself or anyone else, about how well you are recovering. Listen to your body. If it’s telling you to rest, do that. Remember, the fatigue lessens over time, and your strength does return. For me, it took approximately four months.
Don’t Try to push yourself. If you do you might become frustrated and that doesn’t help. In fact it may extend your recovery time.
Pouch Changing 101
I had devised my own schedule for changing the ostomy pouch — every Friday and Monday. A rule of thumb is to change it every three-four days. You will decide what days, how often, as well as choosing a medical supplier that offers products that best suits your needs. After leaving rehab, one company had offered supplies to me. If you, like me, prefer their products, then stick with them. If not, check other distributors and request samples from them. Many people experiment with several companies before finding the products that work for them.
After experiencing a few glitches, (ie; tearing a pouch, or unable to remove the protective piece covering the wafer),you realize some possibly could be avoided in the future. Being aware of these mishaps helps to avoid future problems, and will make the process of changing your bag go more smoothly. In addition, once you have repeatedly gone through this part of your “life without a bladder” it doesn’t require too much thinking or time. Perhaps this thought may be difficult to believe, but it does happen.
Don’t get bent out of shape when things don’t go as planned. Use these experiences as problems to be solved.
You may find other obstacles to overcome. The good news, once these challenges are met and conquered, they make this part of your life more tolerable. It may seem as though you’ll never feel comfortable. The more you are aware of this process, and follow it repeatedly, the easier it is to make the required adjustments. Those who have traveled along this path can be very helpful. They have been for me. The more information you receive, the less stress you will experience.
Be patient with yourself don’t hesitate to ask any questions you may have.
Yes, there are adjustments to make and new roads to travel. Through knowledge gained from resources, along with your own experiences, make this continuing journey just another routine part of your life. However, it takes time and effort. HAVE PATIENCE!!
It has been several years since my surgery. I have learned a lot, and have made adjustments to my life. You can reach this point as well.
YES, THIS IS SOMETHING YOU NEVER EXPECTED. YES, THERE ARE ADJUSTMENTS YOU WILL NEED TO MAKE. YES, THIS PROCESS TAKES TIME. YES, THIS WILL BECOME ANOTHER ROUTINE PART OF YOUR LIFE.
A Second Opinion Leads to a Life-Changing Ostomy
 In the spring of 2014, I had completed another colonoscopy for my ulcerative colitis. It was my fifteenth colonoscopy in twelve years and many prescriptions of drugs later to curtail the bleeding of the polyps in my intestine.
In the spring of 2014, I had completed another colonoscopy for my ulcerative colitis. It was my fifteenth colonoscopy in twelve years and many prescriptions of drugs later to curtail the bleeding of the polyps in my intestine.
I had a very productive career and life with a CPA practice for 34 years. In Grapevine, Texas I served on the school board and as a city council member, and was named “Citizen of the Year.” But bleeding and bathrooms were getting on my nerves, so I called the Mayo Clinic in Rochester, Minnesota, unbeknownst to my gastro doctor. I told them that I wanted another opinion.
After four days of extensive tests, discussions, colonoscopy, the doctors at Mayo concluded that the polyps were entirely too large to remove by minor surgery without bigger risks, and that removal of my large intestine was recommended. Cancer was discussed at length including risks and possibilities with large polyps and various medical unknowns involving my circumstances.
My large intestine was removed January 4, 2015. The surgery was in my home town and I had a great ostomy nurse that taught me all of the intricacies of the ostomy pouch and supplies. I returned to retirement life again here in the Mountains of Texas where it is cool in the summer and we return to Grapevine for the winter where we had our careers.
I am 76 today and walk with my dog 3 to 10 miles each day. I play golf anytime I can. I am very active in my small town and I play the organ at our church each Sunday. I am not overweight and enjoy eating most anything. I find it necessary to chew every piece of food very well. I avoid nuts, corn, kale, popcorn, and tough fruit skins.
I love life and I am so happy for the decisions I made.
Saturday, October 3rd, 2020 marks the 10th anniversary of Ostomy Awareness Day. In partnership with United Ostomy Associations of America (UOAA), Hollister Incorporated is proud to stand with the entire ostomy community in celebration. Every ostomate has a voice worth hearing and we aim to embody ostomy confidence of our worldwide community with #OstomateVoices.
Spread Positivity and Share Your Voice

We’re connecting and empowering our worldwide ostomy community to share their own unique experiences—their challenges, their achievements and the joys of their daily lives. Share your words of encouragement that have helped you along your ostomy journey. Your story might help someone who might be struggling. Using your words, we’ll create a unique social card that you can share with your friends, family, and community. Share your voice here!
Join Us for a Virtual Cooking Class

Join us for a virtual cooking class on October 3rd with private chefs Ryan Van Voorhis, a fellow ostomate, and Seth Bradley of Nude Dude Food™, one of Chicago’s most sought after private dining and catering services. Register today to connect with others in the community and cook a delicious meal. Register today!
For more resources on nutrition with an ostomy, check out UOAA’s Food Chart or download the “Eating with an Ostomy” Nutrition Guide.
Show Off Your Stoma Sticker

Stoma stickers are a great way to raise awareness, start a conversation, or show support. Order your free Stoma Stickers in time for Ostomy Awareness Day, shipped anywhere in the US.
Share a photo or video of your Stoma Sticker on social media using #StomaSticker to be part of the conversation. Or show off your Stoma sticker while running in your virtual Run for Resilience Ostomy 5K and share how you celebrated #OstomyDay2020.
Share your #OstomateVoices and personalize your next Instagram or Facebook Stories with the Hollister “Ostomate Voices” digital stickers. It’s easy – search “Ostomate Voices” in the GIF library when creating a Story and you’ll find the whole collection, including a UOAA lifesaver and Stoma Sticker!
For more resources and interactive ways to get involved, visit Hollister.com/ostomyawareness.
Editor’s Note: this blog post was provided by Hollister Inc. the exclusive Diamond Sponsor of UOAA’s annual Run for Resilience Ostomy 5K events that benefit UOAA, a 501(c)(3) nonprofit organization.
A Decade of Shining a Positive Light on Lifesaving Ostomy Surgery
By Jeanine Gleba, UOAA Advocacy Manager
“Ostomates Unite and Help Place The Ostomy In A Positive Light! Celebrate UOAA’s Ostomy Awareness Day!” These were the words that were spread when UOAA announced the first National Ostomy Awareness Day on July 25, 2010. A decade later, UOAA continues to sponsor and celebrate this day annually in the United States by raising awareness about this life-saving surgery and increasing national visibility of those living with ostomies. Starting in 2014, and all subsequent years, UOAA has been celebrating Ostomy Awareness Day on the first Saturday of October, which coincides with World Ostomy Day every three years. This year National Ostomy Awareness Day will be held on Saturday, October 3, 2020.
The idea for an awareness day was originally suggested by Ally Bain, who worked with UOAA as a summer intern in 2010. (Flash forward, this is the same Ally instrumental for the Restroom Access Act (aka Ally’s Law). The awareness day began as an experiment in social media to see what kind of grassroots support they could get for ostomy recognition. UOAA sent out a request on social media asking all followers to show their allegiance to the cause by changing their online status to the slogan above and make their profile picture UOAAs logo. The immediate response was so strong that they were also contacted by friends at Talkin’ Bout Guts, to host a 24-hour live podcast in honor of ostomy awareness. Thousands participated that year.
In recent years, UOAA has also named an Ostomy Awareness Day Champion. This year’s champion is Robin Brown, pageant winner Mrs. Washington, who uses her stage platform to raise awareness for ostomy surgery “all in the hopes that it can be a light for someone stumbling in the darkness”. Her ostomy story and journey from farm girl to the title of Mrs. Washington World America is inspiring. Watch her special video message for Ostomy Awareness Day!
Over the years, celebrations have been centered around several different themes including Bouncing Back into Life, Navigate the Journey Together, Speaking Out Changes Lives and, most recently, Ostomies Are Life-Savers.
To commemorate the 10th anniversary, here are 10 ways you can join the movement to raise ostomy awareness this year:
- Help shine a positive light on ostomy surgery and go “live” on your own at 7:00PM EDT on October 3rd with people all across the United States. Hit the “live” button on your personal social media accounts (Facebook, Instagram or TikTok) to shine a light on yourself and tell everyone how your ostomy saved your life or that of a loved one. If you are a medical professional, share how your work helps save lives.

- Participate in our 7th annual Run for Resilience Ostomy 5k. This year our local Ostomy 5k events will be held virtually along with our annual worldwide virtual Run/Walk, so you can walk or run in your favorite place or at home. Visit www.ostomy5k.org to register or donate for one of these events. You can also join UOAA’s “United Advocates Smashing Stigma” team too!
- Create a fundraising team through one of our Ostomy 5k events and challenge your family, friends, Affiliated Support Group members, colleagues and coworkers to raise ostomy awareness and funds for a good cause! Have your teammates share the team campaign and see who can get the most donations. Better yet, ask your employer to match any donations raised!
- Make a donation to the “Ostomy Awareness Fund” as a tribute to the 10th anniversary. Donate a minimum of $30 and receive a special bandana with the “Ostomies Are Life-Savers” graphic image. These bandanas are also a great pet accessory. Share a photo with UOAA of your pet raising ostomy awareness!

- Participate in some of the events we have planned with partners such as the Facebook Live Event that will be co-hosted with Crohn’s and Colitis Foundation on October 3rd.
- Raise awareness and spread the message that ostomies are life-savers using our infographic. We encourage you to share, post or print it wherever possible.
- Our Operation Ostomy – A Life Saver campaign continues to spread the message that we are saving lives one ostomy at a time. Please use our 10th Anniversary Ostomy Awareness Day logo for your profile picture on your social media accounts. Use the hashtags: #OstomiesAreLifesavers #OstomyDay2020 and tag UOAA on Facebook @uoaainc Instagram @uoaa_ or Twitter @uoaa.
- Get your Federal, State or Local elected officials to pass a proclamation declaring October 3, 2020 as the 10th anniversary of this special day. Use our sample proclamation or take action here.
- Use our sample letter to the editor to share with your local media why ostomies are life-savers.
- Aside from Ostomy Awareness Day, October is full of fun fall activities. Carve a pumpkin (or paint) in an ostomy theme. “Shine a light” in your carved pumpkin and raise ostomy awareness in your neighborhood.
For more information and the latest ways to get involved including activities from some of our sponsors visit https://www.ostomy.org/ostomy-awareness-day/.
With your help we will carry on breaking the silence and shining a positive light on what has saved so many lives.
Contact Us

United Ostomy Associations of America
P.O. Box 2293
Biddeford, ME 04005-2293
Call us toll-free at: 1-800-826-0826.
Our Information Line hours are Monday-Friday, 9am to 3pm EST. If you have an emergency, please dial 911 or contact your local medical professional.
Please understand that UOAA is a private, nonprofit, advocacy and informational organization. We are not a medical facility and we do not have medical or legal professionals on staff. Therefore, UOAA does not provide Medical, Mental Health, Insurance or Legal Advice. Visit UOAA Virtual Ostomy Clinic provided by The Wound Company for non-emergency, virtual ostomy support.
Get Involved
UOAA is the leading organization proactively advocating on behalf of the ostomy community. Recognizing that we are always stronger together, we encourage everyone to get involved by joining our Advocacy Network. We’ve also created several Advocacy Tools and Resources to help you successfully advocate on behalf of the ostomy community to ensure every ostomate receives quality care.



