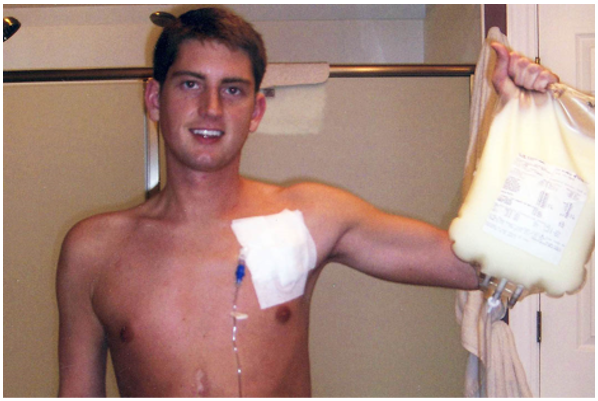
Since short bowel syndrome is not something most people talk about every day, I am excited that we have a month to bring awareness to it. As someone living with short bowel syndrome (SBS) and an ostomy, I have learned to be grateful for the technologies and doctors who have helped keep me alive through my surgeries and infections. And I am proud of myself for developing the self-reliance to find ways to make my life easier.
| To learn more about SBS, visit https://sbs-whattoknow.com/. To join the community and talk with others who are living with SBS, check out https://www.facebook.com/TakedaSBS/. |
People with ostomies come from all stages of life, and we all have different stories to tell. But we also share some common experiences—and we can learn from each other. I have an ostomy because of SBS, a rare digestive disorder that many people may not know much about. If you asked me about my memories of my SBS diagnosis, I couldn’t answer that because I don’t remember it. My SBS diagnosis happened right after I was born. Fortunately, my doctors quickly ran tests and diagnosed me with Hirschsprung’s disease, a condition at birth where certain nerves are missing from parts of the intestine. I immediately had surgery to remove my colon and half of my small intestine, which led to my SBS diagnosis and having an ostomy.
My parents, who were graduate students at the time, were as ready as they could be to bring home a baby, but I think they had prepared for the predictable, everyday challenges of having a “normal” baby, not for me. After my surgery, I spent about one month in the NICU, where the nurses instructed my parents on how to care for me.
When my parents brought me home, they raised me to never feel different and didn’t see my condition as something to hold me back; they wanted me to be independent, which I am! My health condition has been just a part of who I am. I grew up getting hooked up to IV nutrition, a form of parenteral support or PS, every night. It was such a part of my routine that I didn’t know any different. SBS was just part of my life.
From a very early age, I learned how to take care of myself because that’s what parents teach their children. If I hadn’t had SBS, they would have potty-trained me. Instead, they taught me how to drain my ostomy. Their attitude was, This is going to be difficult, but she has to do this. So, we would work on the steps together. Just like other kids learning to make it to the toilet, I learned how to change my ostomy so that I would be ready for school.
Starting preschool was an adventure. How many schools are equipped to care for a kid with an ostomy? Wildly enough, the director of the preschool was an older woman who had friends with ostomies, so she was familiar with my needs! It’s a great example that, despite age differences, we can connect through our ostomy knowledge and help each other out. Eventually, the preschool teachers and director trained the staff at my elementary school when it was time for me to start my education.

As I was growing up, all my friends knew that I had a health condition. I also think I was lucky in that, while I was technically very sick in the beginning, the doctors were able to address it early on. That meant that even though I had a rare digestive disorder, I was actually not a very sick child. Plus, I just didn’t have that concept of shame. For show-and-tell, I’d pull up my shirt to show everyone my line for my parenteral nutrition. And they’d all be like, “Cool! There’s some weird plastic thing hanging out! Moving on…” No one cared.
Then, when I was in middle school, we moved from California to the East Coast. For the first time ever, I had to share my condition with others—in a student population hundreds of times larger than the tiny magnet school I’d left behind. Plus, my health condition started flaring up for the first time. I missed the first day of school due to my first-ever line infection. At that point, I hadn’t really processed what my medical condition meant for my life.
So, I was dealing with complex new health issues while trying to pretend I was “normal.” I got through middle and high school through sheer determination. While I enjoyed my time at school, I often felt like an outsider—like I couldn’t tell people about my true self. I shrank into myself and let fear cause me to lose who I really was. I realized, for example, that the type of shirt “everyone was wearing” would show my line. If I wore the “in” jeans, which were low-waisted, my ostomy bag popped out. I was already not like everybody else just by my clothes alone. Add in missing a lot of school due to hospitalizations and infections, and people would recognize me as “the girl that’s gone all the time.” I let go of hobbies, friends, talents, and dreams just to blend in.
These days, more than two decades after my SBS diagnosis, I don’t worry about blending in so much. Instead, I am clear about my needs, and I’ve figured out what works for me. It doesn’t matter if my jeans are on trend—feeling good and confident in my own skin and my own life matters most. From my clothing choices to creating an ostomy station in my bathroom that’s both functional and cozy, I have learned to set up the things I need to feel comfortable and happy. This also means that when something is stressful or hard, like if the bag breaks in the middle of the night, I already have a bag ready on my nightstand so that I can deal with the issue. I try to think through what might happen when I am clear-eyed and calm so that when difficulties arise (which, in my experience, they have), I can focus on fixing the problem.

I’ve been managing my ostomy on my own since high school, and even when I’m in the hospital or being visited by nurses at home, I take charge of changing my bag. Sometimes the nurses are curious to see how a patient does it independently. I think that as they watch me, they pick up tips and strategies to show their patients different—but still medically acceptable—ways of managing their bags at home. We (or our caregivers) learn the correct procedures in the hospital, and we all find ways to adapt to SBS.
Thankfully, hospitals and homes are two separate things. So when I bring my SBS home with me, I try to be a good host and make it cozy and comfortable.
In recognition of Short Bowel Syndrome Awareness Month, I would like to encourage my fellow SBS patients and their caregivers to stand up and become their own best advocates. As I said, people with ostomies come from all stages of life, and while every patient is unique, we are all in this together.
This article was created by Takeda.
Editor’s Note: This educational article is from one of our digital sponsors, Takeda. Sponsor support along with donations from our readers like you help to maintain our website and the free trusted resources of UOAA, a 501(c)(3) nonprofit organization.

 The seatbelt wrapped around my waist and caused me to lose blood flow to my intestines, which then had to be removed. I was left with no absorptive function and diagnosed with SBS. Though some people may arrive at an SBS diagnosis as a result of other gastrointestinal (GI) conditions, my introduction to SBS was abrupt. One day I was a college basketball player and homecoming king. The next I woke up in the ICU being told I would likely never eat or drink again.
The seatbelt wrapped around my waist and caused me to lose blood flow to my intestines, which then had to be removed. I was left with no absorptive function and diagnosed with SBS. Though some people may arrive at an SBS diagnosis as a result of other gastrointestinal (GI) conditions, my introduction to SBS was abrupt. One day I was a college basketball player and homecoming king. The next I woke up in the ICU being told I would likely never eat or drink again.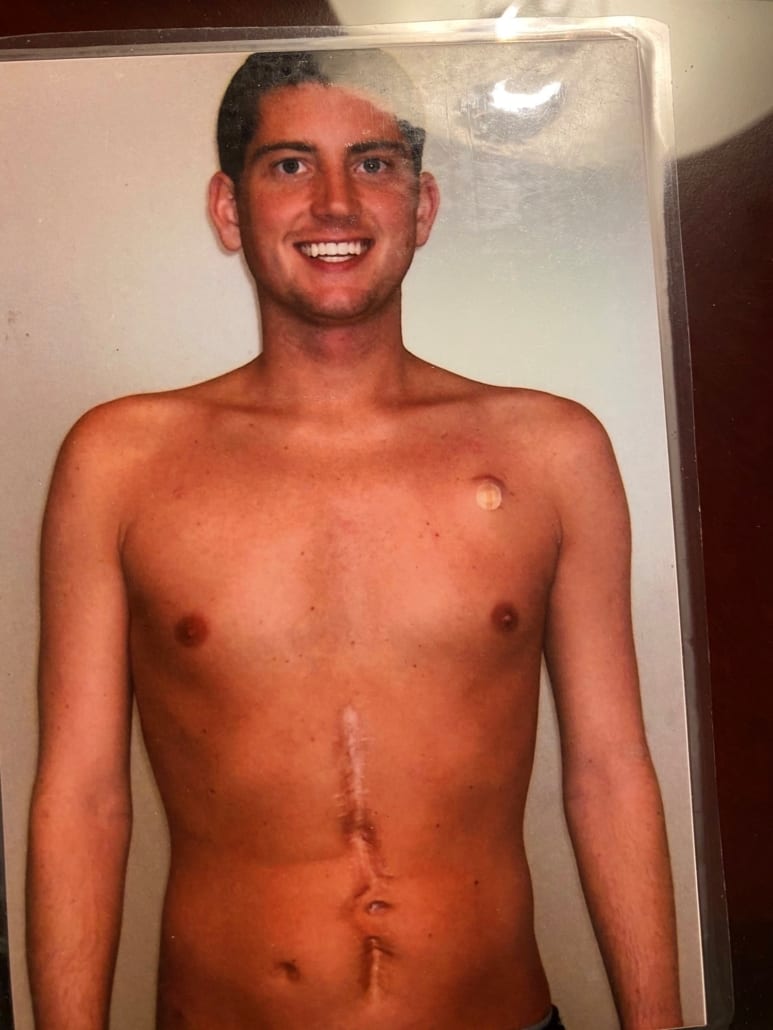 journey! But despite triumphing over those physical challenges, I had more hurdles to face, particularly in terms of my mental and emotional health.
journey! But despite triumphing over those physical challenges, I had more hurdles to face, particularly in terms of my mental and emotional health.