At sixteen, I got my first job doing janitorial work at an amusement park. As you might imagine, I wasn’t thrilled by the work, which included cleaning the restrooms. I remember coming home and complaining to my mother that I wanted to quit. Although I didn’t realize it at the time, her response would soon take on important meaning for me and the way I would approach the rest of my life. She said, “No, honey, you can’t quit. Our family does NOT quit.”
Her message of perseverance was never more critical than following the moment that changed my life forever – a turning point that resulted in my diagnosis of short bowel syndrome (SBS), a serious and chronic malabsorption disorder. Since that moment, I have had to show up for myself every day and make the decision to never quit.
In October of 1999, during the summer between my sophomore and junior years of college, my family’s car was hit head on in a two-lane highway when someone crossed the center line and struck us. I was in the backseat with my then-girlfriend (who is now my wife) buckled in with a lap belt when we were struck.  The seatbelt wrapped around my waist and caused me to lose blood flow to my intestines, which then had to be removed. I was left with no absorptive function and diagnosed with SBS. Though some people may arrive at an SBS diagnosis as a result of other gastrointestinal (GI) conditions, my introduction to SBS was abrupt. One day I was a college basketball player and homecoming king. The next I woke up in the ICU being told I would likely never eat or drink again.
The seatbelt wrapped around my waist and caused me to lose blood flow to my intestines, which then had to be removed. I was left with no absorptive function and diagnosed with SBS. Though some people may arrive at an SBS diagnosis as a result of other gastrointestinal (GI) conditions, my introduction to SBS was abrupt. One day I was a college basketball player and homecoming king. The next I woke up in the ICU being told I would likely never eat or drink again.
The accident left my wife similarly injured — and also diagnosed with SBS — while my mom and stepdad also suffered injuries. Following the accident, our family church would bring food to the house to help out, only I couldn’t eat it. Seeing those casseroles had always been a sign of care, but in those early moments it was torturous. Getting the care I needed early on was a struggle – so much so that my grandma, an amazing supporter of mine, was one of the first people to step in and learn how to administer my total parenteral nutrition (TPN). I’ve been on TPN every night since then.
Due to my SBS diagnosis, for nearly two years, I also needed a jejunostomy, which is an opening created through the skin into the jejunum (part of the small intestines) that can be used for a feeding tube or as a bypass during bowel resection. The sudden need for an ostomy was difficult to accept at first, as I adjusted to my new life with SBS. As time went on and I finally became a bit more comfortable with my ostomy, I remember landing an interview for an internship I really wanted. However, I was so nervous during the interview that my sweat actually caused my ostomy to leak. Although I got the internship, which was a big step towards my personal goals, the experience was a learning curve in becoming confident in the balancing act I’ve had to develop over the years.
I was able to have the ostomy reversed before my college graduation and even graduated on time – a huge victory in the early stages of my SBS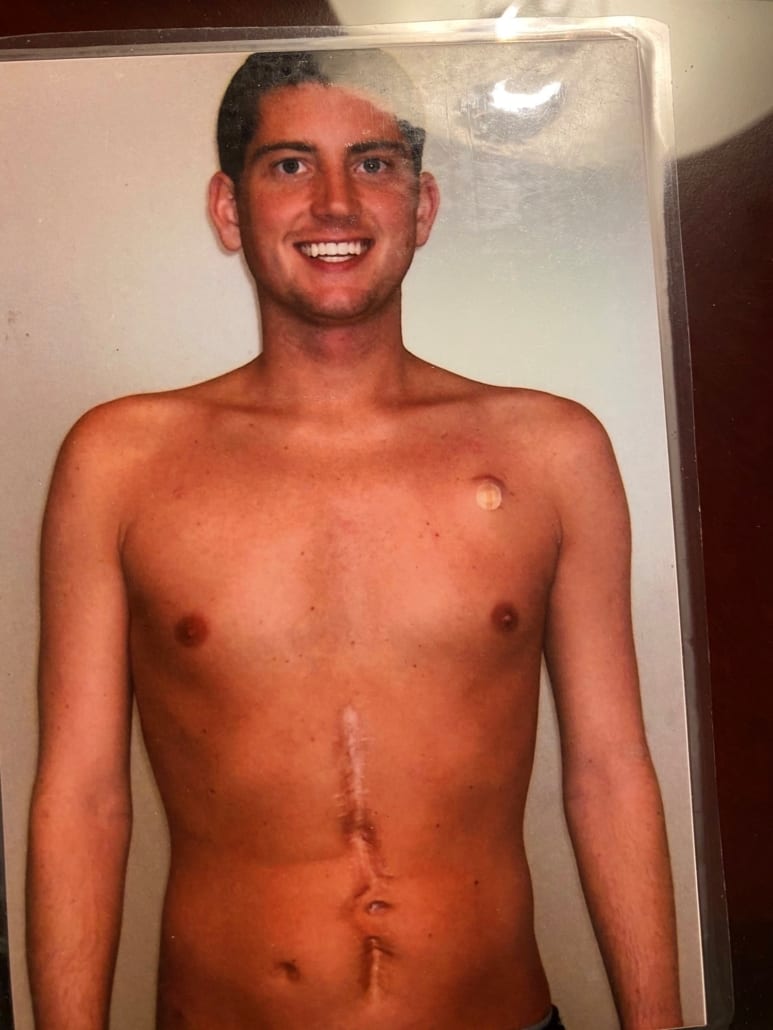 journey! But despite triumphing over those physical challenges, I had more hurdles to face, particularly in terms of my mental and emotional health.
journey! But despite triumphing over those physical challenges, I had more hurdles to face, particularly in terms of my mental and emotional health.
For so long I had identified myself as a basketball player, an athlete, and in a single moment I was told that I would never play again. I cannot describe how devastating that was to hear. I wanted to fight, to call on the determination that had been a large part of my high school and college athletic career, but it was so hard to have that motivated mindset after being blindsided by a diagnosis of a rare disease.
Understandably, I was completely down in the mud for the first few months. I would lie in bed watching movies for hours because facing my reality was too heavy. After months of watching others live out their lives in those movies, I decided that I needed to stop avoiding the fight. I decided that, just as I had trained as an athlete, I now needed to train myself to live. I knew I had to focus on what I could control, lean into the discomfort and push through the obstacles to live life on purpose. Something I’ve come to call “living an intentional life.”
My decision to adopt an intentional mindset and train myself to live turned small steps into monumental milestones. The first thing I tasted after those initial months without any food at all was a red cherry Life Saver candy (ironic, right)? That was my small step. When I tried to make the leap to solid food, I admittedly pushed too far, too fast. Doctors told me that I could eat three bites of food, that was all. So, I bought myself a six-inch Subway sandwich, cut it into three pieces, and ate it in three bites! Regrettably, this wasn’t great for my digestive system at the time. But, it was a learning experience and it felt like progress to me.
To the disbelief of my doctors, and others around me, this shift in my mindset – my transition from victim to victor – translated to my physical health as I began to make steady progress. Nevertheless, I experienced challenges as I navigated how to best advocate for myself and balance my SBS management goals with my personal goals for living my best life.
It took a while to understand which types of care were best for me and the way I wanted to live my life. I am very thankful for my wife, who is a wonderful advocate, registered nurse and fighter. She is the one who was first able to step in and say, “No, this is not acceptable,” when working with my care team. It was hard at times to identify the right care solutions. For example, I initially had a Hickman (or central line), but the wires meant I couldn’t swim or shower. Both were too important to me to give up. Since I do not need to access my port for most of the day, I chose to have a high access port (chest level) that I can access each night instead of a central line that would interfere with my daily routine.
Adjusting to the new port was yet another obstacle, as I need to access it via needle. At first, I would get so nervous every night before that needle stick and I would just cry. But I am grateful I can trade that small amount of time each night for the ability to hold onto some important parts of my pre-SBS routine when I’m not hooked up throughout the day. For example, I remember how happy I was to take my first shower, something that I used to take for granted. I definitely used up all the hot water in our house that day!
These adjustments taught me to accept that I was not invincible and to instead focus on what I can control, taking small steps each day and forming habits to benefit me and my health. Though I have been on TPN every night since the accident, my TPN has evolved and is no longer my only source of nutrients. Now I take in ~30% of my nutrition from food and ~70% from TPN. I’ve also learned that sufficient levels of sodium and hydration are important, so now I salt everything and use lots of hydration tablets.
With my doctors’ support, I was able to start running again. In the beginning, I started with a few steps. Over time, I build up to just one mile each day. Then, I slowly built myself up to two miles, then three. Now, I have completed five half marathons! I continue to swim and play basketball, some of the things I worried I had lost forever because of my SBS diagnosis – I am so grateful they are still a part of my life.
I am also fortunate that my workplace includes a supportive team made up of healthy, go-getters who share similar mindsets to mine when it comes to living an intentional life. This work environment has encouraged me to meet my personal goals, including starting my own financial advising firm. Living with SBS can make the workday uncomfortable and unpredictable. But I establish boundaries and habits that set me up for success, such as the ability to avoid having meetings first thing in the morning or right after lunch when I might need to step away to manage gastrointestinal issues associated with my SBS. And my assistant is a great support in that area. Having those people in your life who have your back is everything.

Self-motivation is big for me, but connecting with others in the SBS community has been motivational in a different way. My wife and I went to advocacy group conferences early on, and I found it encouraging to hear from others with SBS. For example, a man who had been living for 55 years on TPN while continuing to thrive and take control of his journey inspired me to share my own story in hopes that others will see how it is possible to still live a great life with SBS.
I have experienced some very deep lows in my SBS journey, particularly in the beginning, but have learned to embrace the victories. I’ve even faced death, on one occasion in a very close call due to a staph infection near my port. It had brought my blood pressure down to 15/10 and forced the doctors to remove the port immediately. Yet, I’ve also seen the beauty of life – I have witnessed the first breaths of my children and so much more. I truly love life, and these experiences only further solidify my faith and perseverance.
This is a journey of ups and downs, but the downs don’t last. I believe we are not given more than any of us can handle, and I know that I can handle so much more than I ever thought I could. My faith, the blessings I have experienced in my life and the support of my care team, family and many others have brought me back to life. I would encourage anyone living with or caring for someone with SBS to be transparent about the challenges they may be facing and embrace them. Find opportunities within the obstacles and be intentional with your life.
To learn more about Short Bowel Syndrome (SBS), visit https://www.shortbowelsyndrome.com/. To join the community and talk with others who are living with SBS, check out https://www.facebook.com/TakedaSBS.
This article was created by Takeda.
Editor’s Note: This educational article is from one of our digital sponsors, Takeda. Sponsor support along with donations from our readers like you help to maintain our website and the free trusted resources of UOAA, a 501(c)(3) nonprofit organization.






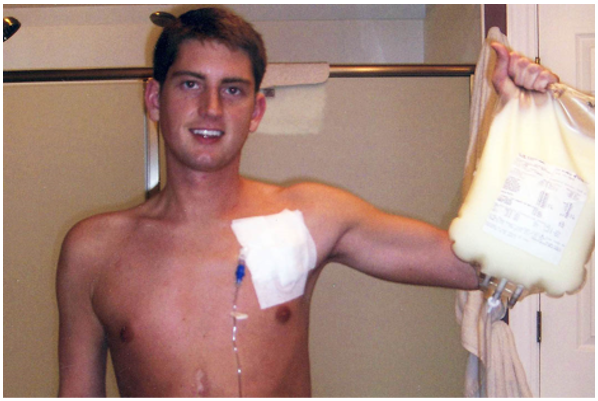
 TPN nourishes my body with the nutrients it’s not capable of absorbing on its own. It’s delivered via a Hickman catheter in the upper left part of my chest, infusing through a pump stored in a backpack while I sleep.
TPN nourishes my body with the nutrients it’s not capable of absorbing on its own. It’s delivered via a Hickman catheter in the upper left part of my chest, infusing through a pump stored in a backpack while I sleep.





 The seatbelt wrapped around my waist and caused me to lose blood flow to my intestines, which then had to be removed. I was left with no absorptive function and diagnosed with SBS. Though some people may arrive at an SBS diagnosis as a result of other gastrointestinal (GI) conditions, my introduction to SBS was abrupt. One day I was a college basketball player and homecoming king. The next I woke up in the ICU being told I would likely never eat or drink again.
The seatbelt wrapped around my waist and caused me to lose blood flow to my intestines, which then had to be removed. I was left with no absorptive function and diagnosed with SBS. Though some people may arrive at an SBS diagnosis as a result of other gastrointestinal (GI) conditions, my introduction to SBS was abrupt. One day I was a college basketball player and homecoming king. The next I woke up in the ICU being told I would likely never eat or drink again. journey! But despite triumphing over those physical challenges, I had more hurdles to face, particularly in terms of my mental and emotional health.
journey! But despite triumphing over those physical challenges, I had more hurdles to face, particularly in terms of my mental and emotional health.

 My journey with Short Bowel Syndrome (SBS) spans 61 years, and it has been full of twists and turns. I’ve often wished that I understood from the beginning exactly what it meant to have SBS – it is not temporary, rather it is chronic. That means it’s a lifelong condition, and it has frequently caused me to make adjustments to maintain my independence and lead a productive and meaningful life. Reaching independence and self-reliance took years of learning the importance of self-advocacy to get the information I needed from my healthcare providers, no matter how difficult it may have been to hear that information. Each symptom, diagnosis, ostomy and medical procedure that preceded my eventual SBS diagnosis posed new challenges. The more I knew about what lay ahead for me, the more I could take charge of my own life. As August marks SBS Awareness Month, I hope my experiences will help inform and inspire others living with this serious and chronic malabsorption disorder to speak up and ask for information and tips to help maintain as much independence as possible.
My journey with Short Bowel Syndrome (SBS) spans 61 years, and it has been full of twists and turns. I’ve often wished that I understood from the beginning exactly what it meant to have SBS – it is not temporary, rather it is chronic. That means it’s a lifelong condition, and it has frequently caused me to make adjustments to maintain my independence and lead a productive and meaningful life. Reaching independence and self-reliance took years of learning the importance of self-advocacy to get the information I needed from my healthcare providers, no matter how difficult it may have been to hear that information. Each symptom, diagnosis, ostomy and medical procedure that preceded my eventual SBS diagnosis posed new challenges. The more I knew about what lay ahead for me, the more I could take charge of my own life. As August marks SBS Awareness Month, I hope my experiences will help inform and inspire others living with this serious and chronic malabsorption disorder to speak up and ask for information and tips to help maintain as much independence as possible. Six years later, I found myself unable to eat due to severe abdominal pains and a pseudo-obstruction and was put back on TPN. I feared this would prevent me from traveling on a three-week family trip to Australia, but my husband and daughters learned how to properly store, prepare and administer my TPN infusions, so we could still travel. I am so grateful to have been able to enjoy that trip with my family despite my TPN, ostomy and needing to use a catheter.
Six years later, I found myself unable to eat due to severe abdominal pains and a pseudo-obstruction and was put back on TPN. I feared this would prevent me from traveling on a three-week family trip to Australia, but my husband and daughters learned how to properly store, prepare and administer my TPN infusions, so we could still travel. I am so grateful to have been able to enjoy that trip with my family despite my TPN, ostomy and needing to use a catheter. 

