 https://www.ostomy.org/wp-content/uploads/2025/07/Blog-image-Body-Image-After-Ostomy-Surgery-Coloplast.png
550
1000
Contributor
https://www.ostomy.org/wp-content/uploads/2017/02/UOAAlogofinal2.png
Contributor2025-07-30 11:06:512025-07-30 11:06:51Navigating Body Image After Ostomy Surgery
https://www.ostomy.org/wp-content/uploads/2025/07/Blog-image-Body-Image-After-Ostomy-Surgery-Coloplast.png
550
1000
Contributor
https://www.ostomy.org/wp-content/uploads/2017/02/UOAAlogofinal2.png
Contributor2025-07-30 11:06:512025-07-30 11:06:51Navigating Body Image After Ostomy SurgeryUrostomy (Urinary Diversion): A surgically created opening in the abdominal wall through which urine passes. A urostomy may be performed when the bladder is either not functioning or has to be removed. There are several different types of surgeries, but the most common are ileal conduit and colonic conduit.
Reasons for surgery: Bladder cancer, spinal cord injuries, malfunction such as chronic infection of the bladder and birth defects such as spina bifida.
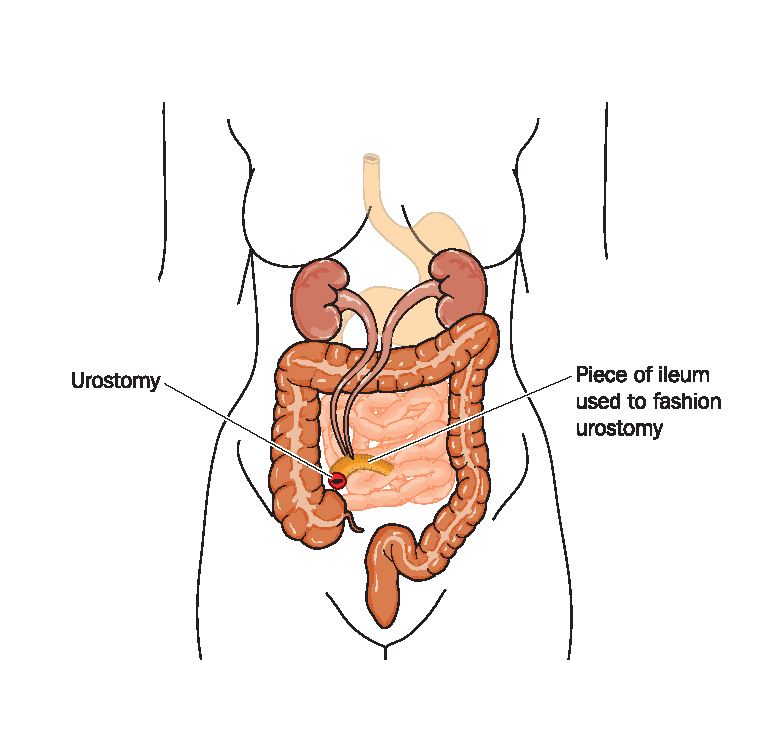
Care of Urostomy
A pouching system is worn. Pouches are odor free and come in many different types to fit your body contours, personal preferences and lifestyle. Ostomy supplies are available at medical supply stores and through the mail and are covered by most health insurance plans.
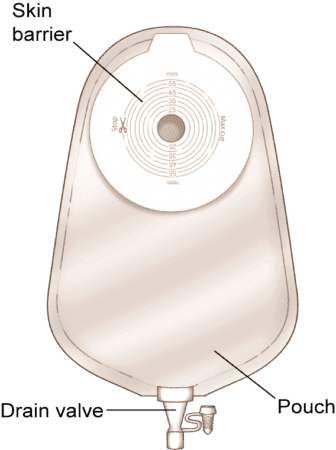
One-Piece Urostomy Pouch
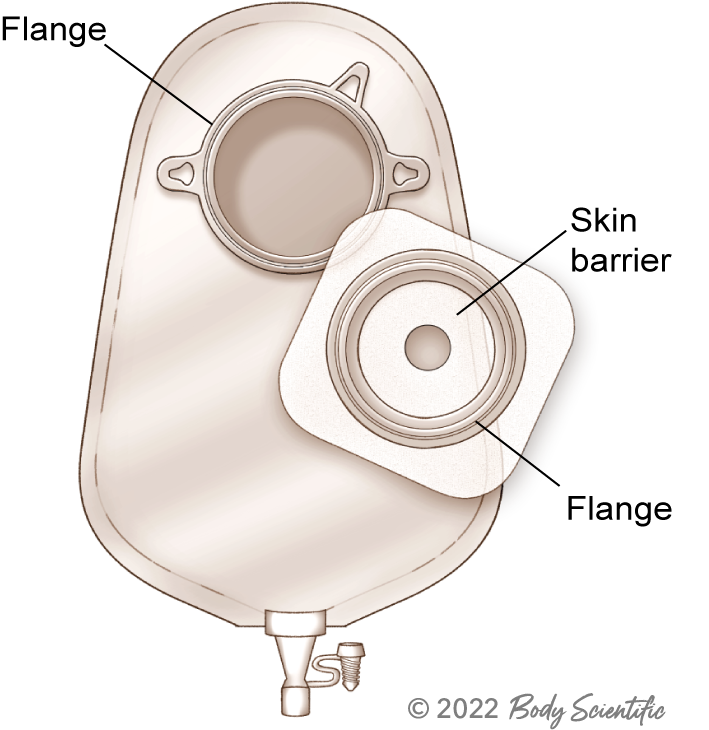
Two-Piece Urostomy Pouch
Living with a Urostomy
Work: With the possible exception of jobs requiring very heavy lifting, a urostomy should not interfere with work. People with urostomies are successful business people, teachers, carpenters, welders, etc.
Sex and social life: Sexual function is influenced by the reasons for which the urostomy is performed. The urostomy itself should not interfere with normal sexual activity or pregnancy. It should not prevent one from dating and continuing relationships and friendships. UOAA Affiliated Support Groups are available for individuals and partners seeking emotional support.
Clothing: Usually one is able to wear the same clothing as before surgery including swimwear.
Sports and activities: With a securely attached pouch one can swim and participate in practically all types of sports. Caution is advised in heavy body contact sports and a guard or belt can be worn for protection. Travel is not restricted in any way. Bathing and showering may be done with or without the pouch in place.
Diet: Usually there are no dietary restrictions and foods can be enjoyed as before. It is suggested that 8-10 glasses of fluid per day be consumed to help decrease the chance of kidney infection.
Sleep: Night drainage systems are available to collect and store urine so can sleep without having to empty your bag multiple times during the night.
Resources available:
Physicians and medical professionals are the first sources of help. Specially trained nurses called Wound, Ostomy and Continence Nurses (WOCN) or Ostomy Management Specialists (OMS) are available for consultation in most major medical centers and some community hospitals.
Read Our Latest Posts About Urostomies:
 https://www.ostomy.org/wp-content/uploads/2025/07/Blog-image-Body-Image-After-Ostomy-Surgery-Coloplast.png
550
1000
Contributor
https://www.ostomy.org/wp-content/uploads/2017/02/UOAAlogofinal2.png
Contributor2025-07-30 11:06:512025-07-30 11:06:51Navigating Body Image After Ostomy Surgery
https://www.ostomy.org/wp-content/uploads/2025/07/Blog-image-Body-Image-After-Ostomy-Surgery-Coloplast.png
550
1000
Contributor
https://www.ostomy.org/wp-content/uploads/2017/02/UOAAlogofinal2.png
Contributor2025-07-30 11:06:512025-07-30 11:06:51Navigating Body Image After Ostomy Surgery https://www.ostomy.org/wp-content/uploads/2023/05/Bladder-cancer-blog.png
808
1149
Contributor
https://www.ostomy.org/wp-content/uploads/2017/02/UOAAlogofinal2.png
Contributor2025-07-13 14:15:282025-07-28 16:07:18UOAA is Here for Bladder Cancer Survivors
https://www.ostomy.org/wp-content/uploads/2023/05/Bladder-cancer-blog.png
808
1149
Contributor
https://www.ostomy.org/wp-content/uploads/2017/02/UOAAlogofinal2.png
Contributor2025-07-13 14:15:282025-07-28 16:07:18UOAA is Here for Bladder Cancer Survivors
Ostomy Anxiety: Horror in the Grocery Store?
Colostomy, Emotional Health, Ileostomy, Ostomy Basics, Ostomy Tips, Personal, Urostomy, Young AdultContact Us

United Ostomy Associations of America
P.O. Box 2293
Biddeford, ME 04005-2293
Call us toll-free at: 1-800-826-0826.
Our Information Line hours are Monday-Friday, 9am to 3pm EST. If you have an emergency, please dial 911 or contact your local medical professional.
Please understand that UOAA is a private, nonprofit, advocacy and informational organization. We are not a medical facility and we do not have medical or legal professionals on staff. Therefore, UOAA does not provide Medical, Mental Health, Insurance or Legal Advice. Visit UOAA Virtual Ostomy Clinic provided by The Wound Company for non-emergency, virtual ostomy support.
Get Involved
UOAA is the leading organization proactively advocating on behalf of the ostomy community. Recognizing that we are always stronger together, we encourage everyone to get involved by joining our Advocacy Network. We’ve also created several Advocacy Tools and Resources to help you successfully advocate on behalf of the ostomy community to ensure every ostomate receives quality care.




