Two ostomy community leaders discuss effective ways to stay positive when times get tough.
Living through a crisis is hard for anyone, but there is an extra layer of concern for people with ostomies. Hollister sat down with two influential people in the ostomy community to find out how they cope during challenging times.
Amber Wallace is the creator of the Ostomy Diaries YouTube channel and social media platforms, and Dr. Paul Wischmeyer, MD is a critical care, perioperative, and nutrition physician at Duke University School of Medicine in Durham, North Carolina. Both Amber and Paul live with an ostomy.
Q: How can people with ostomies stay healthy both physically and emotionally when facing a crisis?
Amber: The best way to take care of your emotional health is to take care of your physical health. Continue to take your supplements. Stick to a schedule and make checklists. During a difficult time, I do the same things at the same time every day and that helps. It’s also important to get enough rest and exercise, even if you have to find a routine online. Grief and anxiety can manifest physically if you don’t put those things into practice.
Paul: I agree with taking the proper supplements. Some of us with ostomies absorb vitamins differently, so it’s important to consult your doctor before starting a regimen. Exercise is also very important. As a senior in college, I was doing research with a doctor at Mayo Clinic. One day he said, “Paul, you’re getting soft and look a little out of shape – do you want to keep getting sick? You should start running and taking better care of yourself.” I had never had anyone say that before and was motivated (and a little miffed) so I started running and ran almost every day for a year. And when that same doctor performed my tenth surgery to remove my failed ileal pouch, it took only four hours instead of eight. Afterwards he said, “Your abdomen looked like you never had surgery – your adhesions were gone! Whatever you did in the last year, you should definitely keep it up!” I haven’t stopped running and exercising since.
Q: What can we do to stay healthy if we have to travel during a health crisis?
Amber: It’s important to keep a change of ostomy supplies on your person when traveling and make sure to stay hydrated. We all have leak stories. One time I was hiking in the Great Smoky Mountains and my pouch fell off. I had to change it in a porta potty! And, of course, I use hand sanitizer constantly, especially on my phone.
Paul: I’ve had leaks on planes and have had to run to the washroom with it pouring down my leg. Never a dull moment with an ostomy some days! I keep supplies in a small kit. I also always wear an ostomy belt, which helps keep my pouch secure. When my wife and I travel now we wear masks and bleach wipe everything we have to touch.
Q: Where should people turn when having a really bad day?
Amber: Stay connected with nature and focus on things that are beautiful. Take a moment and be still. Keep grounded and turn to your faith. It’s OK to cry and let those emotions out. Recognize it, feel it, and embrace it. There’s a myth that if you ignore depression it will go away. You have to deal with it before you can move ahead. Last year after my wedding I was feeling down and didn’t know why. I was too ashamed to tell anyone. So I decided to speak to my doctor. He ran some tests and it turned out that my vitamin levels were out of whack. Never be ashamed to talk to your doctor, that’s what they’re trained in.
Paul: Well, as I shared before, exercise has been a true lifesaver for me. When I’m down I also often turn to my family. Being vulnerable is hard especially when you’re sick. I often have trouble loving myself with a body that could turn on me and threaten my life at any moment. Just a few years ago, I was sick again and needed three surgeries and a prolonged hospital stay (almost a month). My wife slept every night at my bedside in the hospital. Through that I realized that perhaps I am loveable no matter what. When feeling depressed, another resource I often use is to connect to the ostomy community on Instagram and other social media. I’ve seen so many people get support from others all over the world. It’s definitely healing to share your story…and to hear others and know you are not alone.
Q: A crisis can present problems with participating in milestone events, such as graduations and funerals. How can people still stay connected?
Amber: If it’s a death, you can honor them by the way you live your life and stay positive. That’s how you can keep their memory alive. If it’s a graduation or birthday, plan something with the person or people when you’re feeling better or the crisis is over. Connection is so important. Check-in with people, even your happy friends. You never know what they’re going through. Gratefulness works too, I write down one thing I’m grateful for each day and put it in a jar.
Paul: I agree about gratefulness. In our family, we play a game every night called “3 GOOD THINGS” where we all go around and name three good things that happened each day. At our hospital, we are spending conscious time thanking people for the little things they do. Getting out of your head and thanking someone else is so essential and therapeutic. It’s so important especially if you’re down. Gratitude is as rewarding to yourself as it is to the one you’re thanking.
This is an excerpt from “Tips for Coping in a Crisis” in the Hollister Incorporated Ostomy Learning Center. Read the full article here.
Editor’s note: This article is from one of our digital sponsors, Hollister Incorporated. Sponsor support along with donations from readers like you help to maintain our website and the free trusted resources of UOAA, a 501(c)(3) nonprofit organization.




 My journey with Short Bowel Syndrome (SBS) spans 61 years, and it has been full of twists and turns. I’ve often wished that I understood from the beginning exactly what it meant to have SBS – it is not temporary, rather it is chronic. That means it’s a lifelong condition, and it has frequently caused me to make adjustments to maintain my independence and lead a productive and meaningful life. Reaching independence and self-reliance took years of learning the importance of self-advocacy to get the information I needed from my healthcare providers, no matter how difficult it may have been to hear that information. Each symptom, diagnosis, ostomy and medical procedure that preceded my eventual SBS diagnosis posed new challenges. The more I knew about what lay ahead for me, the more I could take charge of my own life. As August marks SBS Awareness Month, I hope my experiences will help inform and inspire others living with this serious and chronic malabsorption disorder to speak up and ask for information and tips to help maintain as much independence as possible.
My journey with Short Bowel Syndrome (SBS) spans 61 years, and it has been full of twists and turns. I’ve often wished that I understood from the beginning exactly what it meant to have SBS – it is not temporary, rather it is chronic. That means it’s a lifelong condition, and it has frequently caused me to make adjustments to maintain my independence and lead a productive and meaningful life. Reaching independence and self-reliance took years of learning the importance of self-advocacy to get the information I needed from my healthcare providers, no matter how difficult it may have been to hear that information. Each symptom, diagnosis, ostomy and medical procedure that preceded my eventual SBS diagnosis posed new challenges. The more I knew about what lay ahead for me, the more I could take charge of my own life. As August marks SBS Awareness Month, I hope my experiences will help inform and inspire others living with this serious and chronic malabsorption disorder to speak up and ask for information and tips to help maintain as much independence as possible. Six years later, I found myself unable to eat due to severe abdominal pains and a pseudo-obstruction and was put back on TPN. I feared this would prevent me from traveling on a three-week family trip to Australia, but my husband and daughters learned how to properly store, prepare and administer my TPN infusions, so we could still travel. I am so grateful to have been able to enjoy that trip with my family despite my TPN, ostomy and needing to use a catheter.
Six years later, I found myself unable to eat due to severe abdominal pains and a pseudo-obstruction and was put back on TPN. I feared this would prevent me from traveling on a three-week family trip to Australia, but my husband and daughters learned how to properly store, prepare and administer my TPN infusions, so we could still travel. I am so grateful to have been able to enjoy that trip with my family despite my TPN, ostomy and needing to use a catheter. 





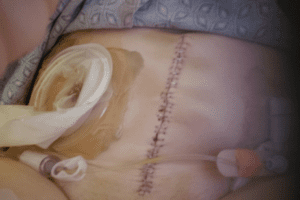 I was not in a great deal of pain which was easily managed with Tylenol. I was definitely weak, but otherwise ok. I went home in 4 days, on my own with my urostomy.
I was not in a great deal of pain which was easily managed with Tylenol. I was definitely weak, but otherwise ok. I went home in 4 days, on my own with my urostomy. Rudolph, my red, round stoma
Rudolph, my red, round stoma

 Night Drainage Pouch
Night Drainage Pouch



